A doctor-supervised weight loss program is a medical treatment for obesity designed and monitored by a licensed healthcare professional, not a commercial diet or self-directed plan. In large medical programs, participants reached a maximum average weight loss of 15.3% from baseline at 4 months, and the average change remained -5.8% at 5 years, which shows that medically supervised care can produce meaningful results that last.
If you're reading this after trying diet apps, cutting carbs, skipping meals, or starting over every Monday, you're not alone. Many adults don't need more internet advice. They need a plan that matches their medical history, their medications, their schedule, and the health conditions that often travel with weight gain, such as diabetes, high blood pressure, sleep problems, or insulin resistance.
That’s where doctor supervised weight loss programs make sense. They turn weight loss from a guessing game into a monitored treatment plan with clear steps, realistic goals, and follow-up. For patients in Maryland, that also means thinking about practical access: local visits, on-site lab work, and telemedicine when getting to the office is hard.
Table of Contents
- What Are Doctor Supervised Weight Loss Programs
- The Five Pillars of a Medical Weight Loss Program
- The Role of Medications Like Semaglutide
- Weighing the Benefits and Risks
- Navigating Program Costs and Insurance
- How to Choose the Right Weight Loss Program
- Frequently Asked Questions and Your Next Step
What Are Doctor Supervised Weight Loss Programs
Doctor supervised weight loss programs are structured medical plans that assess why weight gain is happening, then treat it with nutrition, behavior change, activity guidance, monitoring, and sometimes prescription medication. That’s very different from a meal plan downloaded from social media or a supplement promoted online.
For many people, the most frustrating part of weight loss isn't losing a few pounds. It's losing them, regaining them, then feeling blamed for a problem that may involve appetite regulation, medications, stress, sleep, thyroid disease, insulin resistance, or chronic illness. A medical program starts by asking the right questions instead of assuming every body responds the same way.
A growing number of patients are looking for that kind of credibility. In the medical weight loss services market, 61% of patients prefer physician-supervised programs, and 72% maintain sustainable weight reduction long-term according to market data on medically supervised weight loss services.
Many patients don't fail diets. The diet fails to account for the patient's biology, medications, and daily life.
A simple way to think about it is this:
- A commercial plan gives you general rules.
- A doctor supervised program gives you medical evaluation, follow-up, and treatment changes when the first plan doesn't fit.
- A primary care-based approach can also connect weight treatment to blood pressure, diabetes, cholesterol, sleep, and other ongoing health issues.
If you want a patient-friendly outside explanation of achieving weight loss goals safely, that resource captures the same core point. Safe weight loss usually comes from supervision, not speed.
The Five Pillars of a Medical Weight Loss Program
The strongest doctor supervised weight loss programs don't rely on one tool. They combine several tools that support each other.
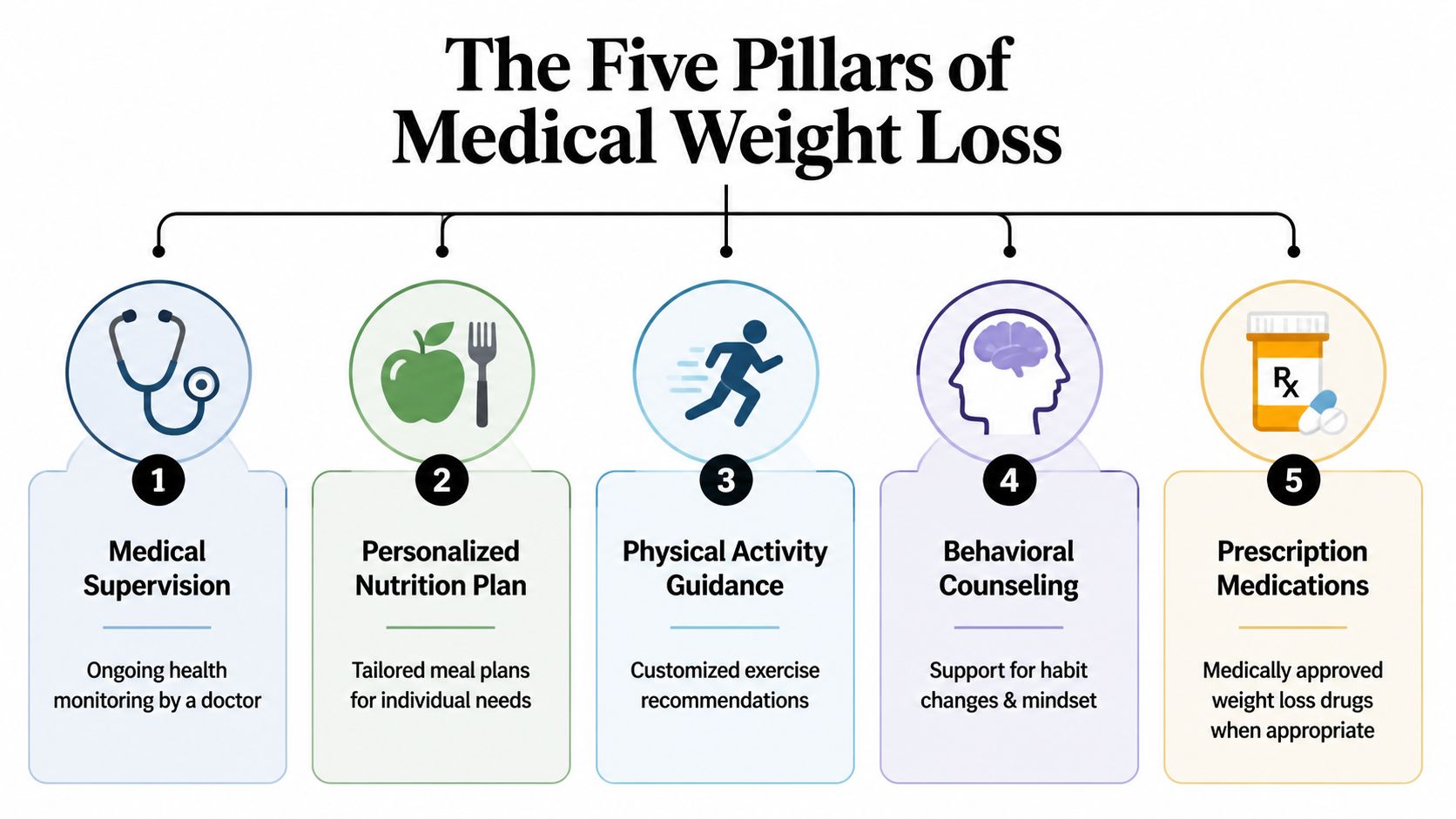
When these parts work together, results are typically better than diet advice alone. A summary of supervised programs reports 15-20% body weight reduction compared with 5-10% from diet-alone approaches in programs that integrate nutrition, medical oversight, and appropriate treatment of underlying factors, as described in this overview of medically supervised weight loss programs.
Medical assessment
The first visit shouldn't be a rushed weigh-in. It should be a clinical evaluation.
Your clinician may review:
- Medical history including diabetes, hypertension, sleep issues, thyroid problems, and past weight-loss attempts
- Current medications because some prescriptions can affect appetite or weight
- Symptoms such as fatigue, cravings, reflux, snoring, or irregular eating patterns
- Labs and baseline measurements to guide safe treatment decisions
For patients already managing long-term illness, weight treatment often works best when it's tied to broader care plans, including chronic disease management.
Personalized nutrition plan
A medical nutrition plan isn't just “eat less.” It considers what you can realistically do.
Some patients do better with structured meal timing. Others need help with late-night eating, portion size, convenience foods, or protein intake. A strong plan should fit your work hours, cooking ability, culture, budget, and health conditions.
Practical rule: If the nutrition plan can't survive a busy week, it probably won't survive six months.
Behavioral counseling
This is the piece many people underestimate. You already know which foods are healthier. The harder question is why eating changes under stress, boredom, poor sleep, grief, travel, or family pressure.
Behavioral support helps patients identify patterns such as:
- All-or-nothing thinking after one “bad” meal
- Stress eating during work or caregiving overload
- Hidden triggers like skipped breakfast leading to evening overeating
- Plateau frustration that causes people to quit too early
Physical activity guidance
Exercise matters, but it has to match your body and your starting point. A patient with knee pain, obesity, and high blood pressure may need a completely different plan than someone who already walks daily.
Good programs usually start with sustainable movement. That may mean walking, resistance work, gentle conditioning, or a home-based plan rather than an intense gym routine you won't keep up.
Medical monitoring and treatment
Monitoring is what turns a plan into medical care. Your clinician tracks progress, reviews side effects, adjusts the strategy, and decides whether medication is appropriate.
That may include changing calorie targets, ordering follow-up labs, reviewing blood pressure or blood sugar trends, or prescribing treatment when lifestyle changes alone aren't enough. This pillar is also where safety lives.
The Role of Medications Like Semaglutide
Medications have changed the conversation around obesity treatment. They haven't replaced nutrition and habit change, but they can make those changes more achievable for the right patient.
What these medications actually do
Drugs such as semaglutide belong to a group often used to reduce appetite, slow stomach emptying, and help patients feel full with less food. Other medications may target appetite in different ways. The right choice depends on medical history, current conditions, side-effect tolerance, and cost.
Used inside supervised care, GLP-1 medications have been associated with 15-20% body weight loss, and early 2026 FDA data cited by UCLA notes that common gastrointestinal side effects were managed 40% faster under physician supervision with access to on-site labs, as described by UCLA’s PRO weight management program.
That point matters because many people hear the success stories but not the practical details. Nausea, constipation, vomiting, dehydration risk, and dose adjustments are not side notes. They are part of treatment.
Why supervision matters
A clinician does more than write the prescription. They decide:
- Whether you're a candidate
- Which medication fits your risks
- How fast to increase the dose
- What to do if side effects appear
- When to stop, switch, or continue
Some patients also ask about pill options and newer medication formats. If that applies to you, a useful local explainer is this overview of oral Ozempic and weight loss medication options.
This short video gives a basic patient view of how medically guided treatment works in practice.
Medication isn't a magic fix. It works best when patients still practice meal structure, hydration, activity, sleep, and follow-up. When those pieces are missing, medication often becomes a frustrating cycle of initial improvement followed by drift.
Weighing the Benefits and Risks
Some patients avoid medical weight treatment because they worry it's extreme. Others expect it to work effortlessly. Neither view is accurate. The actual situation is more balanced, and more useful.

Where the benefits show up
The most important benefit isn't cosmetic. It's clinical.
In a large medically supervised weight program, participants reached a maximum average weight loss of 15.3% from baseline, and despite later regain, the average remained -5.8% at 5 years according to this large-scale study of medical weight management durability. That kind of durability matters because obesity is usually a long-term condition, not a short project.
Patients may also benefit from closer management of conditions that often travel with weight gain. In everyday primary care, that can mean seeing how weight treatment connects with blood sugar, blood pressure, sleep, liver health, and medication burden. If you want to understand one of those links, this overview of obesity and liver health is worth reading.
For people trying to build habits outside the clinic too, this guide on lasting weight loss results is a useful complement to medical care.
What risks patients should understand
Risks depend on the treatment used. Common concerns include medication side effects, frustration during plateaus, unrealistic expectations, and burnout from trying to change too many behaviors at once.
Here's a straightforward comparison:
| Area | Potential benefit | Potential risk | How supervision helps |
|---|---|---|---|
| Nutrition changes | More structure and better intake | Restriction that feels unsustainable | The clinician adjusts the plan |
| Medications | Appetite reduction and better adherence | GI side effects or poor tolerance | Dose changes and monitoring |
| Activity | Better stamina and function | Injury or overdoing it | Exercise is matched to health status |
| Long-term follow-up | Better relapse prevention | Dropout if the plan is too burdensome | Visits are tailored to real-life barriers |
A supervised program doesn't remove every challenge. It gives you someone who responds when the challenge shows up.
Navigating Program Costs and Insurance
You decide you are ready to start. Then the practical questions hit all at once. What will the first visit cost, what happens if labs are needed, and will insurance help pay for any of it?
That uncertainty is common, especially for patients comparing online programs, spa-style weight loss offers, and physician-led care in Maryland. A doctor supervised program often has a few separate cost categories because you are paying for medical decision-making, monitoring, and follow-up, not just a number on a scale.
What you may be paying for
A medical weight loss program works like building a treatment plan in layers. One layer is the evaluation. Another is the monitoring. A third may be medication or nutrition support, depending on what you need.
Depending on the clinic and your insurance plan, your costs may include:
- Initial consultation for medical history, exam, and treatment planning
- Lab work before treatment or during follow-up
- Follow-up visits to review progress and adjust the plan
- Prescription medications if they are part of treatment
- Nutrition or behavioral support if those services are billed separately
That structure can surprise patients who expected a single package price. In a medically supervised program, separate billing is often a sign that the clinic is treating weight care like healthcare, with individual services documented and individualized for the patient.
If you live in Maryland, ask one more practical question early. Can the clinic handle care in a way that fits your schedule? A local practice such as Maryland Primary and Urgent Care may offer a mix of in-person visits, follow-up coordination, and access points that are easier to manage than a distant specialty center. Convenience matters because missed visits can stall progress.
If you have been reading highly restrictive diet advice online, pause before trying it on your own. A public-facing guide for 1000 calorie weight loss can show why very low-calorie plans need medical context, especially if you take prescription medications or have blood sugar concerns.
Questions to ask your insurance plan
A short insurance call before your first appointment can prevent expensive surprises later. General questions often lead to general answers, so it helps to ask about each part of care one by one.
Use language like this:
- Visit coverage: “Is an office visit for obesity or weight management covered under my plan?”
- Provider type: “Does coverage differ if I see a physician, nurse practitioner, or physician assistant?”
- Lab coverage: “Which baseline or follow-up labs are covered when ordered for obesity-related care?”
- Medication coverage: “Are anti-obesity medications covered, and is prior authorization required?”
- Follow-up frequency: “How many follow-up visits for weight management are covered each year?”
- Telemedicine: “Are virtual follow-up visits covered the same way as in-person visits?”
- HSA or FSA use: “Can I use HSA or FSA funds for visits, labs, or prescribed treatment?”
Write down the representative’s name, the date, and any reference number for the call.
That small step helps if the bill you receive does not match what you were told.
How to Choose the Right Weight Loss Program
Not every clinic offering weight loss is offering medical weight loss. Some centers are careful and evidence-based. Others are built around quick enrollment, minimal evaluation, and broad promises.

Questions worth asking before you enroll
Long-term maintenance deserves special attention. A meta-analysis cited by Loma Linda notes that only 28% of supervised participants maintained at least 5% weight loss at 2 years, which means the best programs don't just help you lose weight. They prepare you to keep it off through a medically supervised weight-loss maintenance approach.
Ask direct questions such as:
- Who is supervising the program and how often do I see that clinician?
- What happens if I don't tolerate the first medication or don't want medication at all?
- How do you handle plateaus and regain?
- What is your maintenance plan after the active weight-loss phase?
- Do you provide in-person visits, telemedicine, on-site labs, or coordination with primary care?
For patients in this region, one practical option is Maryland Primary and Urgent Care, which offers adult primary care, on-site lab services, and telemedicine across Maryland, Washington, DC, Virginia, and Florida. That kind of setup can be helpful when weight treatment needs to stay connected to blood pressure, diabetes, or other ongoing care.
Red flags that should make you pause
A few warning signs should slow you down:
- Universal promises if the clinic acts like one plan works for everybody
- No maintenance strategy if all the focus is on the first few months
- No meaningful medical review before prescribing treatment
- Pressure to buy supplements or packages before you've had a proper evaluation
- Little follow-up after starting medication
A good program should sound thoughtful, not flashy. If the sales pitch is louder than the medical explanation, keep looking.
Frequently Asked Questions and Your Next Step
A few questions come up in almost every first visit. Here are the plain answers.
Common questions patients ask
| Question | Answer |
|---|---|
| How fast will I lose weight each week? | It varies. A safe program focuses on steady progress, not forcing the scale down as quickly as possible. Your rate depends on your starting point, medical conditions, nutrition pattern, activity, and whether medication is used. |
| How long do I need to stay in the program? | Most patients do better when they think in phases: active weight loss, adjustment, and maintenance. Obesity usually needs ongoing management, especially if you've regained weight in the past. |
| Can I do this if I have diabetes or high blood pressure? | Yes, and that’s often when supervision matters most. Your clinician can coordinate medication changes, monitor labs, and adapt the plan as your weight and metabolic health change. |
A simple first-step plan
If you're considering doctor supervised weight loss programs, start with three actions:
- Write down your health history including diagnoses, medications, and past attempts that did or didn't work.
- List your obstacles such as cravings, shift work, emotional eating, travel, joint pain, or medication side effects.
- Book a medical consultation instead of starting another unsupervised reset.
The best first goal isn't “lose a huge amount of weight.” It's “get an accurate medical plan.”
A good first appointment should leave you with more clarity than confusion. You should understand your options, the role of labs, whether medication makes sense, what follow-up looks like, and how success will be measured beyond the number on the scale.
If you're ready to take the next step, Maryland Primary and Urgent Care offers adult primary care, urgent care, weight loss support, on-site lab services, and telemedicine for patients in Maryland, Washington, DC, Virginia, and Florida. You can review options and request an appointment on their website, or call the clinic directly to ask about scheduling a weight loss consultation.
