Chronic disease management is an ongoing, collaborative approach to healthcare that helps you manage the symptoms of a long-term health condition, prevent complications, and improve your quality of life through a personalized plan. About 6 in 10 Americans live with at least one chronic disease, so if you've just been diagnosed, you're far from alone.
Getting told you have diabetes, high blood pressure, heart disease, asthma, or kidney disease can make the future feel suddenly smaller. Many patients hear the diagnosis, nod through the visit, then get home and wonder, "What happens now?" That question is exactly where chronic disease management begins.
This isn't about one prescription and a quick follow-up. It's about building a steady plan that fits your real life, your work schedule, your family responsibilities, your meals, your stress, and your goals. As a primary care doctor would tell you in the exam room, the goal isn't perfection. The goal is progress you can maintain.
When people ask what is chronic disease management, the simplest answer is this: it's a long-term partnership between you and your care team. Together, you track symptoms, adjust treatment, catch problems early, and make daily choices that support better health instead of waiting for a crisis.
Table of Contents
- Introduction A New Path to Managing Long-Term Health
- The Five Pillars of Chronic Disease Management
- Chronic Disease Management in Action for Common Conditions
- Your Active Role in Your Health Journey
- How We Support Your Chronic Care Needs in Maryland
- The Proven Benefits of Consistent Management
- Frequently Asked Questions About Chronic Disease Management
Introduction A New Path to Managing Long-Term Health
A chronic condition is a health problem that lasts a long time and usually needs ongoing attention, not a one-time fix. That can sound heavy at first. But in practice, it means you and your clinician create a plan to keep the condition from gradually taking over your day-to-day life.

The need for that kind of care is widespread. Approximately 6 in 10 Americans live with at least one chronic disease, and these conditions are a primary driver of the nation's $4.9 trillion in annual health care expenditures, according to the CDC's chronic disease facts and statistics.
That matters for one reason above all: chronic disease management isn't a niche service for a few patients. It's a core part of modern primary care because long-term conditions are common, serious, and often manageable when people have the right structure.
Practical rule: A diagnosis changes your plan. It doesn't erase your ability to live well.
What chronic disease management really means
A good management plan usually includes regular visits, lab checks when needed, medication review, symptom tracking, and coaching on food, activity, sleep, and stress. It also means your doctor looks at the full picture instead of treating each problem in isolation.
For example, someone with high blood pressure may also be dealing with poor sleep, chronic stress, weight changes, or medication side effects. If those factors aren't addressed, the blood pressure number on the chart may never improve for long.
Why patients often feel confused at first
Individuals don't struggle because they "don't care." They struggle because the advice feels fragmented.
- Too many instructions: You may hear about diet, exercise, medications, home monitoring, and referrals all in one visit.
- No clear priority: Patients often don't know what to do first once they leave the office.
- Real-life barriers: Work hours, childcare, transportation, and medication costs affect follow-through.
- Silent symptoms: Some conditions, especially hypertension, may not feel urgent even when they are.
Chronic disease management solves that by turning scattered advice into a clear, ongoing plan.
The Five Pillars of Chronic Disease Management
Some patients think disease management means "come in more often." That's only a small part of it. A better way to picture it is a house that stays standing because several supports work together.
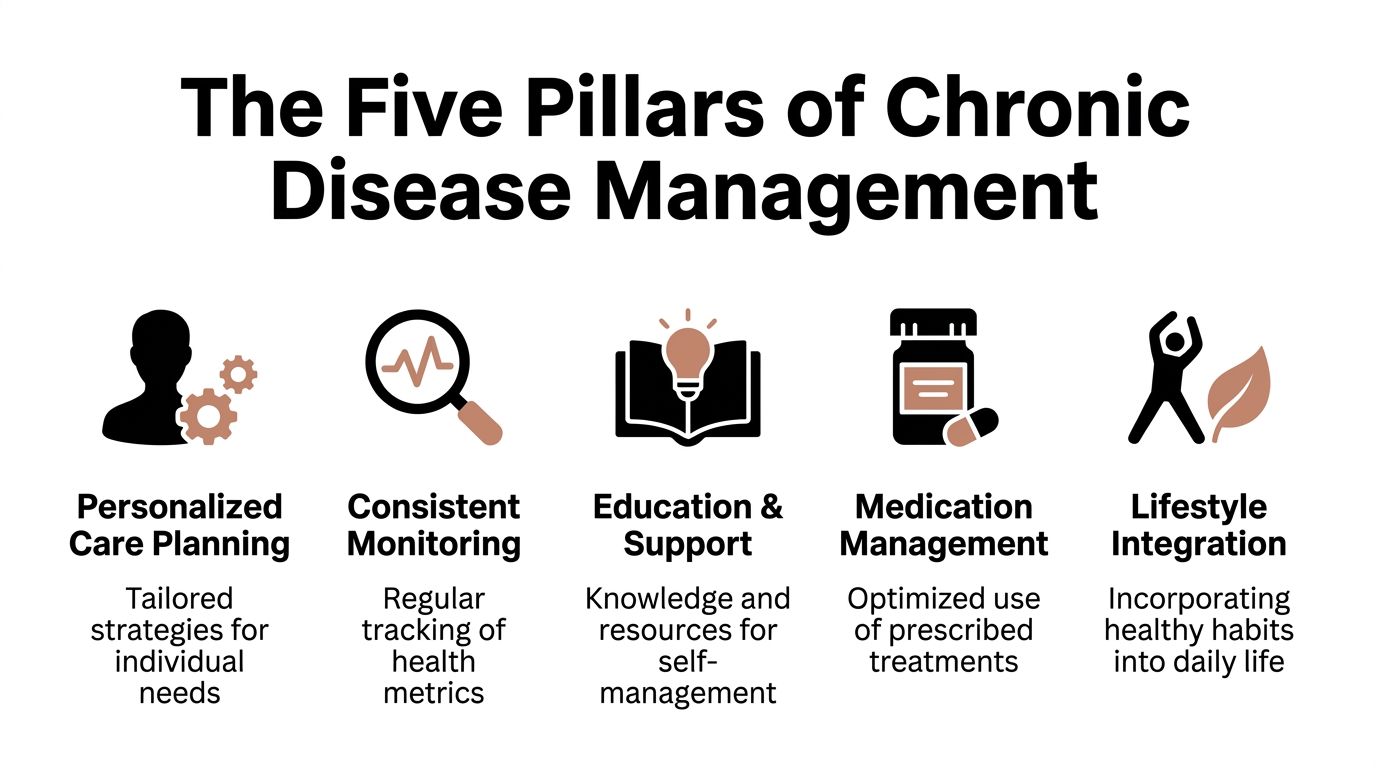
A simple way to think about the process
If one pillar is weak, the whole plan becomes harder to sustain. You might have the right medication but no follow-up. Or you may be motivated to eat better but not understand what your lab results mean.
That's why strong chronic disease care usually includes these five pillars.
Personalized care planning
Your plan should match your diagnosis, medical history, routines, and goals. Two people with diabetes may need very different strategies depending on their work schedule, eating patterns, or other conditions.Consistent monitoring
This includes blood pressure checks, glucose logs, symptom updates, or lab work at the right intervals. Monitoring isn't busywork. It shows whether your condition is staying stable or drifting in the wrong direction.Medication and treatment management
Many patients need help understanding what each medication does, when to take it, and what side effects to report. This is where on-site pharmacist counseling can support clearer medication use and better follow-through.Lifestyle education and support
This pillar is where advice becomes practical. "Eat healthier" is too vague. Patients need specific guidance on meals, movement, sleep, and daily habits they can maintain.Coordinated care communication
If you also see a cardiologist, endocrinologist, nephrologist, or therapist, someone needs to keep the full picture organized. Good communication prevents confusion, duplicate testing, and mixed messages.
Good chronic care doesn't ask you to manage everything alone. It gives you a system.
The five pillars at a glance
| Pillar | What It Involves |
|---|---|
| Personalized Care Planning | A care plan built around your condition, history, goals, and daily life |
| Consistent Monitoring | Regular tracking of labs, symptoms, vital signs, and warning signs |
| Medication Management | Reviewing prescriptions, timing, side effects, and adherence barriers |
| Lifestyle Education and Support | Coaching on food, physical activity, sleep, stress, and routines |
| Coordinated Care Communication | Making sure all providers and follow-ups work together clearly |
Chronic Disease Management in Action for Common Conditions
The idea becomes much easier to understand when you see how it works in real life. The condition changes, but the structure stays the same.
Diabetes in daily life
A patient with diabetes may start with a plan that includes regular blood sugar checks, lab monitoring, medication review, and nutrition counseling. The numbers matter, but the routine matters just as much.
Maybe breakfast is often skipped, lunch is rushed, and dinner happens late after work. In that situation, managing diabetes isn't just about saying "avoid sugar." It's about building meals and medication timing around the person's actual day.
Common parts of diabetes management include:
- Home tracking: Keeping a record of glucose readings and symptoms.
- Medication review: Reporting low blood sugar episodes, stomach upset, or missed doses.
- Food planning: Learning how meals affect blood sugar, not chasing a perfect diet.
- Preventive follow-up: Catching early changes before they become urgent.
High blood pressure that needs steady follow-through
Hypertension often fools people because they don't feel sick. A patient may say, "I feel fine, so I thought I didn't need the medication every day." That's an extremely common misunderstanding.
With blood pressure management, the focus is often on consistency. Home readings, medication adjustments, salt awareness, sleep quality, stress, and follow-up appointments all play a role. If chest discomfort, deconditioning, or mobility issues are also part of the picture, care may overlap with rehabilitation and even resources for managing chronic persistent pain when pain limits movement and makes healthy routines harder to maintain.
The best blood pressure plan is the one a patient can actually follow on an ordinary Tuesday.
Heart disease and recovery that continues at home
Heart disease management usually extends far beyond the event that first brought it to attention. After a diagnosis, patients often need medication review, blood pressure and symptom monitoring, dietary changes, physical activity guidance, and close coordination with a cardiology team.
A patient recovering after a cardiac scare may be afraid to exercise at all. Another may return to normal activities too quickly. Both need coaching, not just instructions.
In heart disease care, your team often watches for:
- New symptoms: Swelling, chest pressure, shortness of breath, or sudden fatigue
- Medication tolerance: Dizziness, cough, or other side effects that make adherence difficult
- Daily patterns: Weight changes, activity tolerance, sleep, and stress
- Communication gaps: Knowing which symptoms should prompt a call right away
The core lesson is simple. Chronic disease management is not one generic program. It's a practical framework adapted to the condition in front of you.
Your Active Role in Your Health Journey
The most effective care plans aren't built only in the exam room. They're shaped by what you notice, what you struggle with, and what matters to you.

What your care team needs from you
You don't need to become your own doctor. You do need to become an active reporter of what's happening between visits.
That means telling your clinician if a medication makes you dizzy, if you're forgetting doses, if healthy meals feel unrealistic, or if stress is driving late-night eating. Those details are not side notes. They are the raw material of a better plan.
A useful patient role often looks like this:
- Track what changes: Symptoms, home readings, side effects, sleep, or swelling
- Bring questions: Write them down before the visit so you don't forget
- Be honest about obstacles: Cost, transportation, language, work shifts, and caregiving all matter
- Name your goal: Better energy, avoiding hospitalization, walking without fatigue, or staying independent
Recent writing on underserved communities also highlights the value of community health workers and culturally responsive support for helping patients manage blood pressure and other chronic conditions while addressing barriers such as food insecurity, housing, stigma, and language needs, as discussed in this overview of sustainable chronic illness support in underserved communities.
Support works better when it fits your life
Patient engagement isn't about being perfectly compliant. It's about making the plan realistic enough to survive a busy week. If you'd like a practical outside perspective, these effective patient engagement strategies explain why communication, trust, and follow-up systems make such a difference.
A short educational video can also make the idea of partnership easier to picture.
If you tell us where the plan breaks down, we can change the plan. That's not failure. That's good care.
Your family, friends, faith community, and local services can matter too. For many patients, health improves when support extends beyond prescriptions and includes reminders, rides, meal help, or someone to walk with in the evening.
How We Support Your Chronic Care Needs in Maryland
Long-term care works best when follow-up is convenient enough that you don't keep putting it off. Access matters. So does timing.

Tools that make follow-through easier
For patients in Lanham and nearby communities, practical tools can remove some of the friction from chronic care. Telemedicine can make medication follow-ups easier. On-site labs can make it simpler to complete testing without extra stops. Home devices can help your care team see what happens between visits instead of relying only on a single office reading.
Modern tools like Remote Patient Monitoring can play a meaningful role here. Using connected devices like blood pressure cuffs or glucose meters, data can be sent to your care team so they can spot trends and intervene early. In cardiac and diabetes care, studies show RPM can reduce care gaps by 15 to 25 percent, as described in this article on the health advantages of remote patient monitoring.
Some practices also use predictive tools to look for patterns that suggest worsening control before a crisis happens. In plain language, that means the team isn't only reacting. They're also watching for signs that your plan needs adjustment.
Why local access matters
For many people, especially those balancing work and family, the hardest part of chronic disease management isn't understanding the diagnosis. It's getting everything done consistently.
That's where services like these become useful:
- Telemedicine visits: Helpful for medication checks, symptom review, and shorter follow-ups
- On-site lab testing: Makes monitoring more practical when labs are part of the plan
- Coordinated primary care: Keeps the full picture together when more than one condition is involved
- Home monitoring tools: Give more accurate day-to-day information than memory alone
Maryland Primary and Urgent Care offers telemedicine and on-site lab services that can support this type of ongoing chronic care for patients in Lanham who need a more workable follow-up routine.
Patients in outer areas and underserved communities may face added barriers, especially when access to interdisciplinary support is limited. In those settings, telemedicine can help bridge distance and keep the care plan moving instead of stalling between appointments.
The Proven Benefits of Consistent Management
Patients often ask if all this structure is really worth it. The short answer is yes, especially when the program is consistent and evidence-based.
What patients often notice first
The first improvements aren't always dramatic. Many people notice fewer urgent setbacks, better understanding of their condition, more confidence with medications, and clearer communication with their care team.
Evidence-based self-management programs have reported improvements in fatigue, shortness of breath, depression, pain, stress, sleep problems, self-reported health, quality of life, and communication with healthcare providers. Those changes matter because they affect everyday life, not just a chart.
Better chronic care often feels less like a big breakthrough and more like fewer bad days in a row.
Why steady care also makes financial sense
The financial side matters too, especially for patients trying to avoid emergency room visits and hospital stays. The Chronic Disease Self-Management Program has been shown to generate an average of $714 per person in savings through reduced emergency room visits and hospital use, with net savings of $364 per participant after program costs, according to the National Council on Aging's summary of CDSMP outcomes.
That doesn't mean every patient will have the same path. It does mean structured chronic care has measurable value.
If you're managing a long-term condition, regular follow-up is one of the most reliable ways to stay ahead of problems. This is one reason regular doctor's office appointments in managing health effectively remain such an important part of primary care.
Frequently Asked Questions About Chronic Disease Management
| Question | Answer |
|---|---|
| How long does chronic disease management last? | It usually lasts as long as the condition lasts. Some plans become less intensive when a condition is stable, but most chronic illnesses still need ongoing review, even when you're feeling well. |
| Does chronic disease management mean I have to come to the office all the time? | Not always. Some follow-ups can happen through telemedicine, while others need in-person visits, exams, or lab work. The schedule depends on the condition, your symptoms, and how stable things are. |
| Is chronic disease management only for severe illness? | No. It's often most useful before a condition becomes severe. Early management helps patients build routines, understand warning signs, and prevent complications instead of waiting until problems become urgent. |
If you're looking for a primary care team that can help you build a practical, personalized plan, Maryland Primary and Urgent Care offers chronic disease management, telemedicine, and on-site support designed to make follow-up easier for patients in Lanham and the surrounding area.
