The best back pain after car accident treatment starts with a prompt medical evaluation, because mid-back pain after a collision has an average yearly incidence of 236 per 100,000 people, the median time to first reported recovery is 101 days, and 23% of patients are still not recovered after one year. Early action matters because the right diagnosis shapes everything that follows, from medication and physical therapy to imaging, referrals, and insurance documentation.
If you're reading this a few hours or a few days after a crash, you're probably asking a very practical question: is this just soreness, or is something more serious going on? That uncertainty is common. Back pain after a collision can come from muscle strain, irritated joints, a disc injury, or a fracture, and those problems don't all feel the same or need the same treatment.
A lot of people make the same mistake. They either ignore the pain because adrenaline masked it at first, or they jump straight to one form of treatment before anyone has clearly identified the injured structure. The faster approach is not always the better approach. Accurate diagnosis first, targeted treatment second is what usually leads to a safer recovery.
Table of Contents
- Why Your Back Hurts After a Car Accident
- How Doctors Diagnose Your Back Pain
- Comprehensive Back Pain Treatment Options
- Expected Recovery Timelines and Self-Care
- Navigating the Auto Accident Clinic Process and Insurance
- How Maryland Primary and Urgent Care Can Help
- Frequently Asked Questions About Post-Accident Back Pain
Why Your Back Hurts After a Car Accident
Back pain after a crash often feels confusing because the symptoms don't always match the damage. Some people feel only stiffness at first. Others get sharp pain when they sit, twist, cough, or try to stand up straight.
The crash force doesn't have to feel dramatic to injure your back
A car accident creates sudden deceleration, rotation, and compression through the spine. Your body stops with the seat belt and seat, but the muscles, ligaments, discs, and small spinal joints absorb the force. That can leave you with anything from a simple strain to a more significant structural injury.

Whiplash doesn't affect only the neck. The same whipping motion can strain the upper and mid-back, especially around the shoulder blades and thoracic spine. If you want a plain-language explanation of the symptom pattern, this guide to understanding whiplash symptoms is useful for recognizing how delayed pain can show up after the initial shock wears off.
Researchers tracking traffic-collision injuries found that mid-back pain had an average yearly incidence of 236 per 100,000 people, the median time to first reported recovery was 101 days, and 23% remained unrecovered after one year in a population-based cohort study published in mid-back pain after traffic collisions research. That's one reason it makes sense to seek care early instead of assuming it will fade on its own.
Common back injuries after a collision
Not every post-accident back injury is serious, but every serious injury starts as "back pain." That's why the details matter.
Muscle strain or ligament sprain
This is common after sudden bracing during impact. Pain is often sore, tight, or spasm-like, and movement makes it worse.Facet joint irritation
These small joints in the spine can become inflamed after twisting or extension during the crash. Patients often describe more localized pain, especially with bending backward or rotating.Disc injury
A bulging or herniated disc may irritate a nerve root. That pattern is different. Pain may shoot into the buttock or leg, and you may notice numbness, tingling, or weakness.Vertebral fracture
This is less common, but it's the problem you don't want to miss. Fracture pain is often severe, focal, and aggravated by standing, walking, or any jarring movement.
Back pain that radiates, causes numbness, or comes with weakness needs a medical exam, not guesswork.
A careful first visit helps put language around your symptoms. If you're deciding what to do next after the collision itself, this step-by-step guide on what to do after a car accident injury can help you organize the medical side quickly.
How Doctors Diagnose Your Back Pain
The first medical visit shouldn't feel rushed or mysterious. A good evaluation usually answers three questions. What happened in the crash, what symptoms followed, and what findings suggest muscle injury versus nerve or bone involvement?
What happens at the first medical visit

The history matters more than many patients expect. A physician will ask where you were hit, whether your car spun, whether airbags deployed, whether you were bracing, and whether symptoms started immediately or later. Those details help narrow the injury pattern.
Then comes the physical exam. The doctor checks posture, range of motion, tenderness, muscle spasm, reflexes, strength, and sensation. If pain shoots down an arm or leg, or if weakness appears on one side, that changes the level of concern.
A proper exam also looks for red flags that don't belong in routine conservative care, including possible fracture, major disc injury, or neurologic compromise.
Practical rule: The first provider should be someone who can triage the full problem, not just treat one possible piece of it.
When imaging changes the plan
Advanced imaging is what separates "probably a strain" from "we know what structure is injured." According to advanced imaging for back injuries after a car accident, MRI has 90 to 95% sensitivity for detecting herniated discs, CT scans have over 95% specificity for identifying bony fractures, and structural injuries like herniated discs or fractures can occur in up to 20 to 30% of moderate-to-severe collisions.
That doesn't mean every sore back needs an MRI on day one. It means imaging is selected based on the exam.
Here is the basic logic doctors use:
| Test | What it helps detect | When it tends to be useful |
|---|---|---|
| X-ray | Alignment problems and obvious fractures | Focal spine tenderness, persistent pain, concern for bony injury |
| CT scan | Detailed bone injury | Strong suspicion for fracture after higher-force trauma |
| MRI | Discs, nerves, ligaments, soft tissue | Radiating pain, numbness, weakness, or symptoms that don't fit a simple strain |
A lot of treatment errors happen when care starts before the diagnosis is solid. Manipulation may help one patient and aggravate another. Rest may help in the first short window but delay recovery if it turns into inactivity for too long.
This short video gives a helpful overview of the kind of clinical reasoning that often goes into spine assessment after trauma:
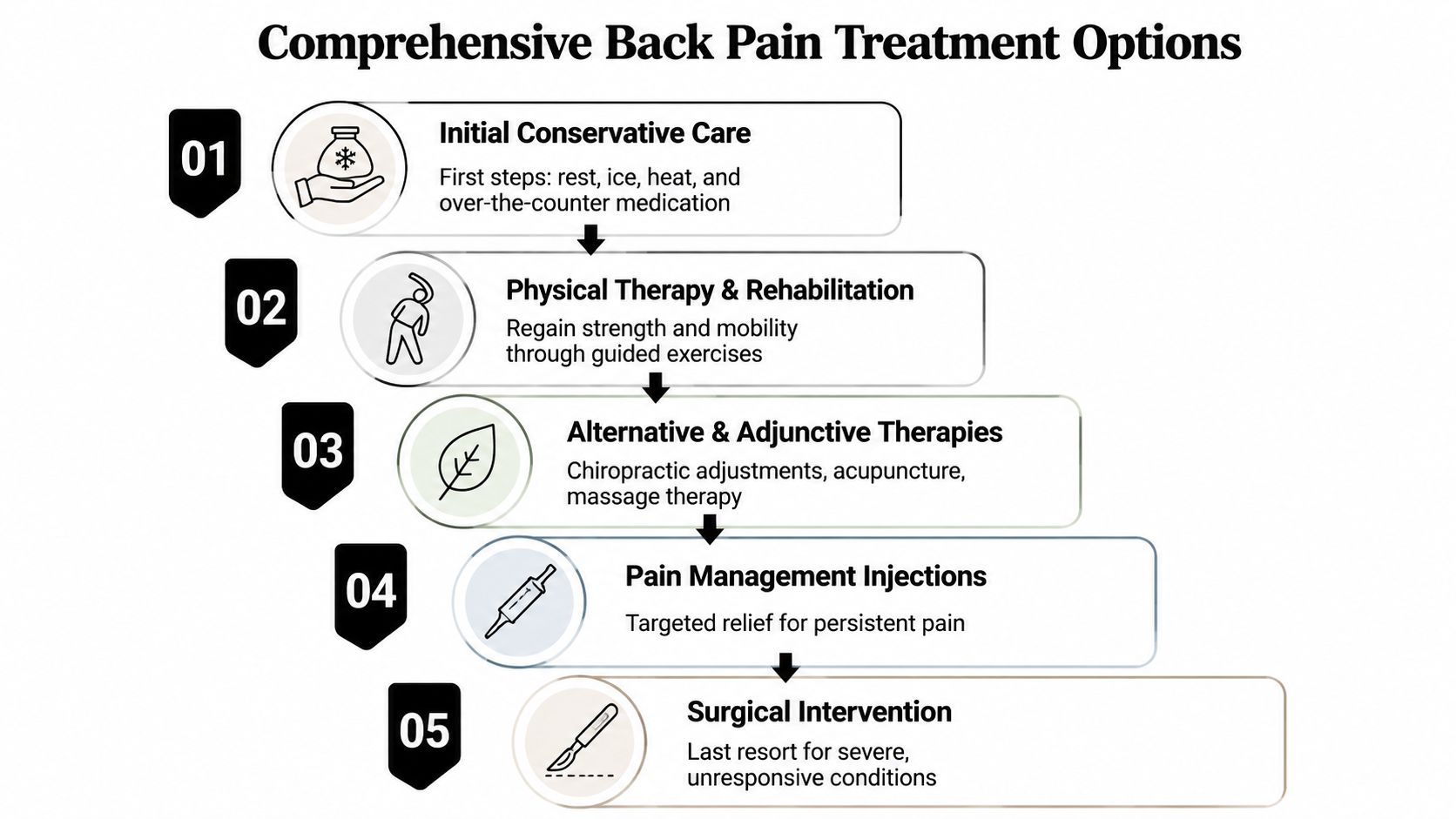
Comprehensive Back Pain Treatment Options
Treatment works best when it follows the diagnosis. That's the central point. The goal isn't to throw every option at the pain. The goal is to match the treatment to the injured tissue, your symptom severity, and how you're functioning day to day.
Start with the least invasive treatment that fits the injury
For many patients, the early phase of back pain after car accident treatment starts conservatively. That may include a short period of activity modification, ice early on if swelling and acute soreness are dominant, then heat later for stiffness and muscle guarding. Over-the-counter anti-inflammatory medication can help some patients, but not everyone should take NSAIDs, especially if they have certain kidney, stomach, bleeding, or cardiovascular issues.
What doesn't work well is a vague "just rest and wait" plan with no follow-up. Too much bed rest often leads to more stiffness, weaker supporting muscles, and more fear of movement. A better approach is relative rest. Avoid the motions that clearly worsen the injury, but stay as gently mobile as your doctor advises.
Some patients also need prescription medication for a short period. That may include a muscle relaxant when spasms are dominant, or other pain-control strategies when sleep and movement are being affected. Medication can reduce symptoms. It doesn't correct biomechanics, rebuild endurance, or identify a hidden disc or fracture.
Where physical therapy, manipulation, and injections fit
Rehabilitation is often where recovery starts to accelerate. Physical therapy focuses on restoring mobility, reducing guarding, and rebuilding support through guided exercise and movement retraining. For post-accident patients, the value is not only pain control but also restoring confidence in normal motion.
There is also good evidence that some combined approaches can help when selected appropriately. In randomized trial evidence on spinal injuries after motor vehicle accidents, combining physical therapy with spinal manipulative therapy led to a 50% greater reduction in pain and a 30% faster return to work compared with medication or rest alone. That does not mean manipulation is right for every patient. It means it can be useful after appropriate medical evaluation has ruled out injuries that need a different path.
If you're comparing rehab approaches, this overview of treatment for whiplash injuries is a practical companion resource because many upper and mid-back injuries overlap with whiplash mechanics.
For persistent pain, care may escalate:
Physical therapy
Best when stiffness, weakness, poor movement patterns, or gradual recovery are the main issues.Spinal manipulative therapy
May help selected patients with mechanical pain patterns, especially when combined with exercise-based rehabilitation.Injection-based pain management
Useful when inflammation or nerve irritation is significant and simpler care hasn't been enough.Surgical consultation
Reserved for specific structural problems such as unstable fractures, major neurologic compression, or pain that matches imaging and fails less invasive treatment.
The right treatment sequence is rarely dramatic. It is usually careful, documented, and adjusted as your exam findings change.
Here is a practical comparison of common options:
| Treatment Type | Best For | Typical Duration / Frequency | Provider |
|---|---|---|---|
| Relative rest, ice, heat | Early pain and muscle spasm | Short-term home care | Patient guided by physician |
| NSAIDs or other medication | Inflammation, pain limiting sleep or movement | Usually short course, based on medical advice | Physician or urgent care clinician |
| Physical therapy | Stiffness, weakness, mobility loss, return to function | Repeated visits over a structured rehab period | Physical therapist |
| Spinal manipulative therapy | Selected mechanical back pain patterns after evaluation | Series of visits based on response | Chiropractor or other trained clinician |
| Injection procedures | Persistent inflammation or nerve-related pain | Usually considered after conservative care | Pain specialist or orthopedic/spine specialist |
| Surgery | Severe structural injury or neurologic compromise | Case-specific | Orthopedic spine surgeon or neurosurgeon |
Expected Recovery Timelines and Self-Care
A reasonable question after diagnosis is, "How long is this going to take?" The honest answer is that recovery depends on what was injured, how severe it is, and how consistently the treatment plan fits the problem.
What recovery often looks like
Some soft-tissue strains improve over weeks. Disc-related pain or more complex injuries can take much longer, especially when sitting, lifting, bending, or driving remain provocative. A more complicated course is also more likely when pain is intense from the start or when the injury affects sleep, work, and concentration.
Research on collision-related low back pain found that several factors predicted a longer recovery, including high initial pain intensity, depressive symptoms, and concentration problems, supporting a broader approach to treatment in this study on recovery and insurance effects after traffic-related low back pain. In practice, that means recovery isn't just about tissue healing. Mood, stress, sleep, and confidence in movement often shape how quickly function returns.
What to do at home without making it worse
Self-care should support the medical plan, not replace it. Keep it simple and specific.
Use movement, not bed rest
Short walks and gentle position changes usually help more than staying in one position for hours.Protect your sitting posture
Keep both feet supported, avoid slumping, and take frequent standing breaks if desk work or driving increases pain.Sleep with support
Many patients do better on their back with a pillow under the knees, or on their side with a pillow between the knees.Track symptom patterns
Note whether pain is local, radiating, numb, or weak. That information helps your clinician decide whether treatment is working or whether the diagnosis needs review.Don't push through nerve symptoms
Sharp shooting pain, worsening numbness, or new weakness during exercise is a reason to stop and check in.
If your home routine leaves you steadily more painful over several days, it isn't the right routine for your injury.
Navigating the Auto Accident Clinic Process and Insurance
The medical part of a crash is only half the problem. The other half is paperwork, timing, and documentation. Many patients feel more stressed by the process than by the treatment itself.
What to do after the crash
Start with the basics. Get medically evaluated, even if symptoms seem delayed or mild. Then keep your paperwork organized from the beginning.

Bring these items to your visit if you have them:
Accident details
Date, location, and a short description of how the collision happened.Insurance information
Auto policy details, claim number if available, and any adjuster contact information.Symptom timeline
Write down when the pain started, what movements trigger it, and whether symptoms are spreading.Prior records if relevant
If you had a previous back problem, bring that information so the physician can separate old issues from new trauma.
If you're unsure why prompt evaluation matters legally and medically, this explanation of why to see a doctor after a car accident lays out the practical reasons clearly.
Why documentation matters as much as treatment
Auto accident care is different from routine urgent care because the chart has to do two jobs. It guides treatment, and it documents the injury in a way insurers can follow.
That means details matter. The note should connect the crash mechanism, exam findings, diagnosis, treatment plan, work limitations if needed, and follow-up recommendations. Missing steps early can create problems later when therapy, imaging, or specialist care needs authorization.
There is also a broader systems lesson here. A landmark study found that when an insurance environment shifted from tort-based compensation to a no-fault system, the median time to claim closure dropped from 505 days to 210 days, a finding discussed in the earlier recovery section's linked study. The practical takeaway isn't about legal theory. It's that efficient claims processes tend to support faster treatment and resolution.
A well-run accident clinic usually helps by coordinating referrals, tracking progress notes, and making sure the record supports the care being recommended.
How Maryland Primary and Urgent Care Can Help
After a collision, patients usually need three things quickly: a careful first evaluation, a clear plan, and follow-through. That's where Maryland Primary and Urgent Care's auto accident clinic is built to help.
The practice offers walk-in urgent care, same-day appointments, and coordinated follow-up for adults dealing with post-accident pain. That matters when symptoms are changing quickly and you don't want to wait weeks for an initial assessment. Dr. Sherif Hassan brings more than 30 years of clinical experience, which is especially valuable when the problem isn't just pain control, but deciding who needs imaging, who can start conservative care, and who should be referred promptly.
The clinic also has practical advantages that fit accident care well. On-site lab services and other in-house diagnostic capabilities make it easier to move from evaluation to documented treatment without unnecessary delays. For patients, that often means less confusion, better continuity, and a more organized paper trail for insurers.
Good back pain after car accident treatment doesn't start with a one-size-fits-all therapy. It starts with a doctor who can sort out what injury is most likely, what needs to be ruled out, and what plan makes sense for the next few days and weeks.
Frequently Asked Questions About Post-Accident Back Pain
Should I go to the ER or urgent care for back pain after a crash
Go to the ER if you have severe weakness, loss of bladder or bowel control, major trouble walking, chest pain, shortness of breath, or a high concern for a major traumatic injury. Urgent care is often appropriate for stable patients with back pain, stiffness, spasm, or delayed symptoms who still need prompt medical evaluation and documentation.
What if my back pain started a day or two later
That happens often. Adrenaline, muscle guarding, and inflammation can delay the full symptom picture. Delayed pain still deserves evaluation, especially if it's worsening, radiating, or interfering with work, sleep, or daily movement.
Should I see a chiropractor first
Not always. For many patients, the safer first step is a medical evaluation that can identify whether imaging or specialist referral is needed before manipulation is considered. Once serious structural issues have been ruled out, chiropractic care may fit into the treatment plan for selected mechanical pain patterns.
Will insurance cover my treatment
Coverage depends on your policy, the claim structure, and the documentation supporting medical necessity. The important part on day one is to get evaluated promptly, report symptoms accurately, and keep all records organized.
When should I worry that this is more than a strain
Be more concerned if pain shoots into the leg or arm, you develop numbness or weakness, the pain is sharply localized over the spine, or basic movement is becoming harder instead of easier. Those findings can point to nerve irritation or structural injury rather than simple soft-tissue soreness.
If you need prompt evaluation and a clear treatment plan, Maryland Primary and Urgent Care provides compassionate care for post-accident injuries with walk-in availability, same-day appointments, and coordinated follow-up to help you move from diagnosis to recovery with less confusion and less delay.
