Monitoring blood sugar at home involves using a glucometer for single checks or a continuous glucose monitor (CGM) that measures glucose every five minutes, and both tools help you manage diabetes, prevent complications, and make better decisions about food, activity, and medication with your clinician. Individuals with diabetes frequently check three to four times daily at common points such as fasting, before meals, two hours after meals, and at bedtime, although the right schedule depends on your treatment plan.
If you've just been told to start checking your blood sugar, you're probably dealing with two problems at once. The first is practical: what device do I buy, when do I test, and how do I do it correctly? The second is emotional: what if I hate finger sticks, what if I forget, and what if every reading makes me anxious?
Both reactions are normal. Home monitoring can feel like one more task added to an already stressful diagnosis, but it usually becomes much easier once you have a routine and understand what the numbers are for. The goal isn't to chase perfection. The goal is to collect useful information that helps you and your healthcare team make safer, smarter decisions.
Table of Contents
- Your Guide to Home Blood Sugar Monitoring
- Why Who and When to Check Your Blood Sugar
- Choosing Your Monitoring Device Glucometer vs CGM
- Mastering the Fingerstick Glucometer Technique
- Interpreting and Acting on Your Results
- Troubleshooting Accuracy Supplies and Advanced Tips
- Frequently Asked Questions About Home Monitoring
Your Guide to Home Blood Sugar Monitoring
A new monitoring plan often starts in a rushed moment. You leave an appointment with a prescription, a few instructions, and a lot of unanswered questions. By the time you get home and open the box, the meter, strips, lancets, and booklet can look more complicated than they really are.
Home monitoring is simpler than it first appears. A blood glucose meter gives a single-point-in-time reading, a snapshot of where your glucose is at that moment. A CGM gives a running stream of information over the day and night. Both can be useful, and neither works well unless you understand how to use the device consistently.

What matters most at the beginning is keeping the process manageable. You don't need a perfect logbook on day one. You need a routine you can repeat without dread.
Practical rule: The best home monitoring plan is the one you'll actually follow when life gets busy, you're tired, or you don't feel like dealing with diabetes that day.
A useful routine has four parts:
- A clear device choice: decide whether you're using a glucometer, a CGM, or both.
- A repeatable testing habit: tie checks to events you already do, such as waking up, eating, or taking medication.
- A basic understanding of the result: know whether you're looking at fasting, before-meal, or after-meal numbers.
- A way to share patterns: keep a written log, app record, or downloaded report for clinical visits.
Many people think monitoring is only about catching a dangerously high or low number. In practice, it's also about seeing how your own body responds. The same breakfast, walk, missed meal, poor night of sleep, or new medicine can affect different people differently. Good monitoring turns guesswork into something concrete.
Why Who and When to Check Your Blood Sugar
Home monitoring changed diabetes care because it moved useful decision-making into the home. The first portable blood glucose meter appeared in 1962, and by the 1980s, devices such as the One Touch could give results in 60 seconds, helping shift diabetes management from the clinic to daily life at home, as described in Cleveland Clinic's overview of blood sugar monitoring.
That history matters because it explains the actual purpose of testing. You aren't checking your blood sugar to satisfy the meter. You're checking so you can see what food, exercise, stress, illness, and medication are doing in real time.
Who benefits from checking at home
Several groups commonly need home monitoring:
- People using insulin: this group often needs the most frequent checks because dosing decisions and safety depend on current glucose data.
- People with type 2 diabetes not using insulin: monitoring may still help, especially when adjusting medications, learning meal patterns, or sorting out symptoms.
- People with gestational diabetes: home readings often help guide treatment and meal planning.
- People with prediabetes or changing risk factors: some clinicians use short-term monitoring to understand patterns, though the plan should be individualized.
If you're also working on broader prevention, adult preventive health screenings often fit into the same conversation because diabetes management works best when blood pressure, kidney health, cardiovascular risk, and routine follow-up are addressed together.
When to check
The right schedule depends on treatment. According to GoodRx guidance on home blood sugar testing, people on diet-only management may test several times weekly, those on insulin shots 1 to 2 times daily may need 1 to 2 tests daily, and those on insulin injections 3 to 4 times daily may need 3 to 6 daily tests. The same source also notes that many people with diabetes commonly check three to four times daily at standard intervals such as fasting, before meals, two hours after meals, and bedtime.
Don't copy someone else's schedule just because it worked for them. Your testing plan should match your medication, your risk of low blood sugar, and how much information you actually need.
Why timing matters
A reading without context is less useful than widely assumed. A blood sugar value means something different if it was taken:
- Fasting, before you've eaten.
- Before a meal, when you're seeing baseline control.
- After a meal, when you're seeing your body's response to food.
- At bedtime, when you're looking for overnight safety.
If you're newly diagnosed, start by learning which moments your clinician wants tracked. That makes your log much easier to understand and much more useful at follow-up visits.
Choosing Your Monitoring Device Glucometer vs CGM
You get home with a new diagnosis, open the supply bag, and realize the hard part is not just learning the equipment. It is deciding what you can realistically keep doing next week, next month, and when life gets busy. The best device is the one you will use consistently enough to guide treatment.
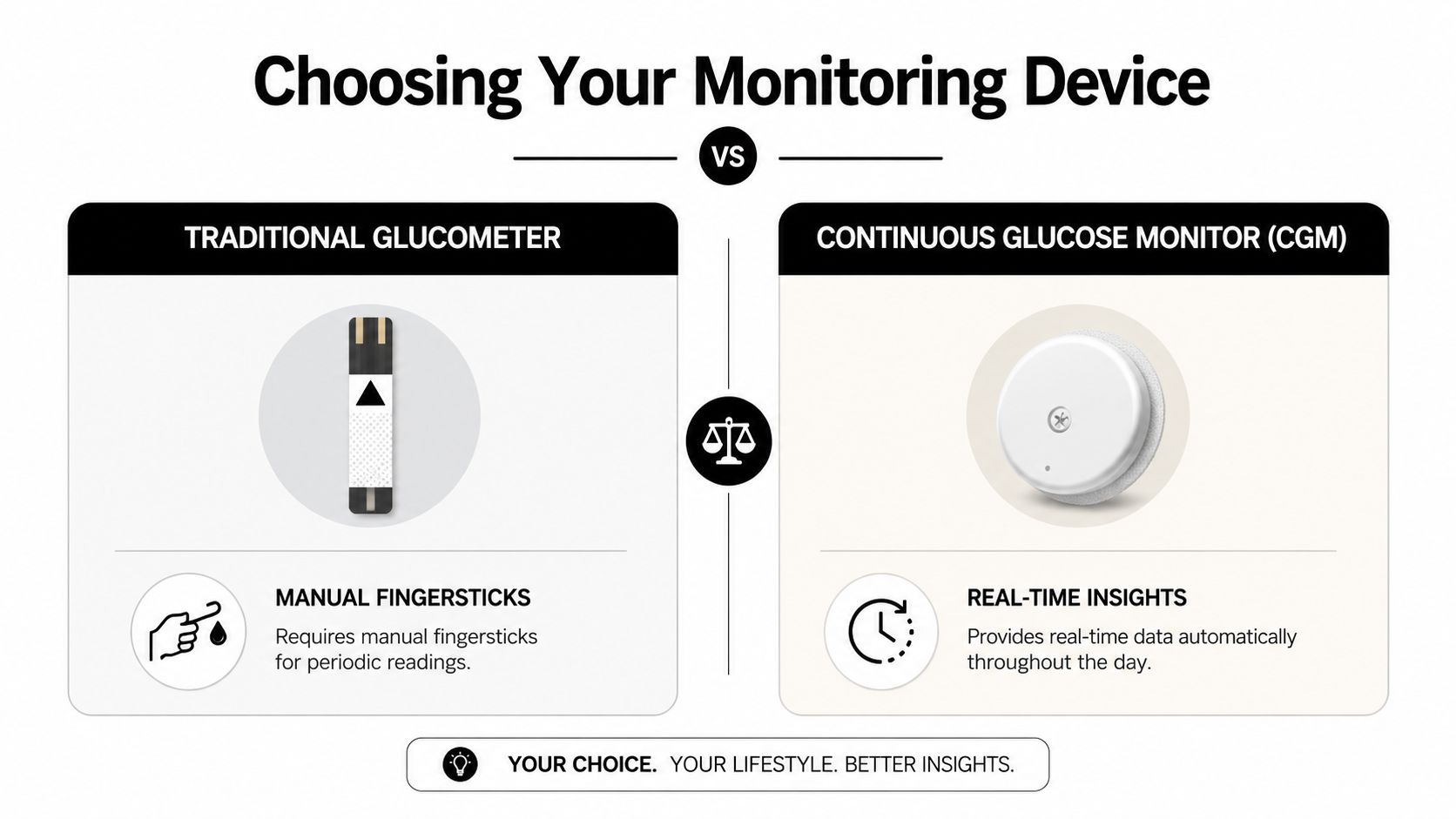
How the two devices differ in daily life
A glucometer gives a single blood sugar reading from a finger stick. It is straightforward, fast, and often the easiest place to start if you only need selected checks at specific times.
A CGM, or continuous glucose monitor, uses a small sensor worn on the body to track glucose levels throughout the day and night. Instead of isolated readings, it shows direction and patterns. That matters if the main question is not just "What is my sugar right now?" but "What usually happens after breakfast, during exercise, or while I sleep?"
The practical difference is bigger than the technical difference. A meter asks you to stop, prepare, prick your finger, and record the result. A CGM reduces that interruption, but it also asks you to wear something on your skin, learn alerts, and tolerate seeing more data.
If you want a broader view of how ongoing home readings can support treatment decisions, this overview of remote patient monitoring for chronic disease care explains how continuous data is used outside the clinic.
Glucometer vs. Continuous Glucose Monitor at a Glance
| Feature | Blood Glucose Meter (Glucometer) | Continuous Glucose Monitor (CGM) |
|---|---|---|
| Type of reading | Single reading from a finger stick | Ongoing glucose trend data from a wearable sensor |
| How often it measures | Only when you test | Repeated readings throughout the day and night |
| What it shows well | Your level at one moment | Patterns, rises, drops, and overnight changes |
| User effort | Manual test each time | Less hands-on checking once the sensor is in place |
| Best for | People who need periodic checks or want a simple setup | People who need pattern data or find finger sticks hard to sustain |
| Main trade-off | Less information between checks | More setup, more alerts, and wearing a device |
Which device fits you best
Choose a glucometer if:
- You want a simple routine: fewer parts, less setup, and a clear job to do at the times your clinician recommends.
- You only need focused readings: for example, fasting checks or occasional tests after meals.
- You do not want a device on your skin: that preference is common and completely reasonable.
- Cost and coverage matter: in many cases, a standard meter is easier to get and maintain.
Choose a CGM if:
- You need to see patterns: this helps when numbers seem unpredictable or symptoms do not match spot checks.
- You are worried about lows, especially overnight: trend information and alerts can add a layer of safety for some patients.
- Finger-prick fatigue is making you avoid testing: reducing repeated sticks can make monitoring more sustainable.
- You feel discouraged by isolated numbers: seeing the full curve often gives better context than a single reading.
The emotional side matters
Many patients assume trouble with monitoring means they are not disciplined enough. Usually that is not the problem. Actual barriers are more ordinary. Sore fingertips. Alarm fatigue. Anxiety after seeing a high reading. Feeling watched by the device. Wanting one part of the day that does not revolve around diabetes.
Those issues should shape the choice.
A glucometer can feel less intrusive because you use it, then put it away. A CGM can reduce pain and guesswork, but some people feel overwhelmed by constant access to their numbers. I often tell patients to choose the device that gives useful information without making them think about diabetes every minute.
Some people use both. A CGM may handle day-to-day trends, while a finger-stick meter is still used in certain situations, depending on the device and the treatment plan. If you are unsure, start with the problem you are trying to solve. Missed checks, unclear food patterns, fear of low blood sugar, or burnout from repeated finger sticks each point toward a different answer.
Mastering the Fingerstick Glucometer Technique
Even people who understand why they need to test often get inaccurate results because of technique. Small mistakes matter. Cold hands, poor strip placement, squeezing too hard, or using supplies incorrectly can turn a useful reading into a misleading one.
Set up before you prick
The standard process includes seven critical steps, from washing hands and using a single-use lancet to safe sharps disposal. The same GoodRx guidance cited earlier notes that fasting blood sugar is typically 60 to 100 mg/dL, many meters measure between 20 and 600 mg/dL, and meters should be checked with control solution weekly and with each new test strip pack for accuracy.
Before testing, make sure you have:
- A working meter: charged or ready to use.
- A test strip: inserted correctly. Some meters won't activate if the strip isn't seated properly.
- A fresh lancet: use a single-use lancet.
- Clean hands: wash with soap and warm water, then dry well.
- A sharps container: don't leave used lancets loose.
Warm water helps because blood flows more easily from warm fingers than cold ones. If your hands are cold, rub them together or let them hang down for a moment after washing.
A clean fingerstick that gives a usable reading
This is the sequence I usually recommend to patients because it reduces frustration:
- Wash and dry your hands fully. Residue on the skin can affect readings.
- Massage the hand gently. This can improve blood flow without forcing blood out.
- Use the side of the fingertip. It usually hurts less than the pad.
- Prick with a single-use lancet. Choose a depth that gives enough blood without excessive pain.
- Apply blood the way your strip requires. Some strips need full coverage of a test area. Others pull blood in from the edge.
- Wait for the result. Most meters display it within seconds.
- Dispose of the lancet safely. Used sharps belong in a sharps container.
A common error is "milking" or squeezing the finger aggressively to produce blood. That often makes the process more painful and can leave you with a poor sample. If you don't get enough blood, it's usually better to pause, warm the hand again, and retry with better technique.
Here's a visual walkthrough if you learn better by watching:
When the meter result doesn't make sense
If a number looks very different from how you feel, slow down before reacting. Ask a few practical questions:
- Did you wash your hands first?
- Was the strip inserted correctly?
- Did the strip get enough blood?
- Are the strips stored properly and current?
- Has the meter been checked with control solution as directed?
If the reading seems wrong, repeat the test using good technique before making a major food or medication decision, unless your symptoms suggest an urgent low or high that needs immediate attention.
The point of learning proper technique isn't to turn testing into a ritual. It's to make each finger stick count so you don't have to keep repeating it.
Interpreting and Acting on Your Results
You check your blood sugar before breakfast and the number is higher than you expected. That can trigger two unhelpful reactions. Panic, or avoidance. Neither helps. A single reading is a clue, not a verdict.

A single number matters less than a pattern
One out-of-range value may reflect stress, poor sleep, illness, a late meal, or timing. Repeated values in the same direction deserve attention because they are more likely to reflect what your body is doing day after day.
CGMs make patterns easier to spot because they collect readings throughout the day and night. Fingerstick testing can still show the same pattern if you check at consistent times and keep a simple record. Three similar fasting readings across several mornings usually matter more than one isolated surprise.
Watch for patterns like these:
- Morning readings that stay high
- Numbers that rise after the same meal
- Lows before lunch or during physical activity
- Bedtime readings that do not fit the rest of the day
This is also where many patients get discouraged. If the numbers are not where you want them, it is easy to feel judged by the meter and start checking less often. I encourage patients to treat the reading like a blood pressure value. It is information you can use, not a grade on your effort.
What to write down every time
A useful log does not need to be detailed enough for a research study. It needs to answer a basic clinical question. What was the number, and what was happening around it?
Write down:
| Record item | Why it matters |
|---|---|
| Date and time | Shows whether the issue happens at a certain part of the day |
| Reading | Gives the actual glucose result |
| Context | Tells whether this was fasting, before a meal, after a meal, at bedtime, or during symptoms |
| Food or missed meal | Helps explain spikes and dips |
| Exercise or unusual activity | Connects movement to glucose changes |
| Symptoms | Shows whether you feel lows or highs reliably |
| Medication timing | Helps your clinician judge whether treatment timing fits your routine |
Paper works. A phone note works. Many meter and CGM apps work. The best system is the one you will still use next month.
If staying organized feels hard, especially when you are also learning medications, meals, and appointments, chronic disease management services can help you review patterns and adjust the plan over time.
How to use the information well
After several days of readings, ask practical questions. Did the high numbers happen after restaurant meals? Did the lows show up on days you were more active? Did fasting readings climb when sleep was poor or when you were sick?
Bring those notes to your appointment. Treatment decisions are better when your clinician can see the setting around the number, not just the number itself.
Patients often assume every unusual result requires an immediate correction. Usually, pattern review is more useful than reacting to one reading in isolation. If the same issue keeps showing up, that may point to meal timing, medication timing, carbohydrate amount, activity, stress, or a need to adjust treatment.
If your results seem unpredictable, that still tells us something important. It may mean the checking times are inconsistent, the daily routine changes a lot, or the current plan does not fit real life very well. That is a problem to solve, not a personal failure.
Troubleshooting Accuracy Supplies and Advanced Tips
Most problems with home monitoring aren't dramatic. They're small, repetitive issues that make the whole process irritating. Strips won't read, the blood drop is too small, the number seems off, or the patient eventually gets tired of doing it. Those are the problems that gradually erode consistency.
Common problems that affect readings
If home checks are frustrating, review the basics first:
- Strip handling: strips need to be inserted correctly, and different brands collect blood differently.
- Hand preparation: dirty or damp fingers can interfere with a clean sample.
- Meter checks: control solution testing matters because accuracy drifts can go unnoticed.
- Supply storage: don't treat strips like loose household items. Keep them where they'll stay protected and easy to find.
- Routine placement: a meter buried in a drawer is a meter that gets skipped.
A practical setup helps more than people expect. Keep the meter, strips, lancets, and logbook in one consistent location. Put them where you normally eat breakfast or take medication. Reducing friction is often more effective than trying to "be more disciplined."
The part many guides skip
The emotional side matters. Research summarized by Mayo Clinic's blood sugar monitoring guidance shows that finger-prick fatigue, testing anxiety, and diabetes burnout can reduce adherence to monitoring schedules.
That means missed checks aren't always a knowledge problem. Sometimes the patient knows exactly what to do and still avoids it. Common reasons include dread of pain, fear of seeing a bad number, shame after an off-plan meal, or simple exhaustion from having to think about diabetes all day.
A few strategies work better than guilt:
- Lower the barrier: keep supplies visible and ready so the task feels shorter.
- Anchor testing to routines: pair checks with breakfast, medication, or bedtime.
- Reduce pain where possible: use the side of the fingertip and review lancet depth.
- Talk about avoidance openly: if you hate testing, say so. That changes the care plan.
- Consider device changes: some people do better with a CGM because it reduces routine finger-stick burden.
Missing readings doesn't mean you're lazy. It often means the monitoring plan doesn't fit your real life yet.
When to contact your clinician
Reach out when a pattern is concerning, when readings repeatedly don't match how you feel, or when you're unsure how to respond safely to highs or lows. You should also contact your clinician if you're avoiding testing because of anxiety, pain, or burnout. That is a medical management issue, not a personal failure.
Persistent uncertainty deserves attention. So does any repeated problem with supplies, technique, or interpretation. The fix is often straightforward once someone reviews your routine with you.
Frequently Asked Questions About Home Monitoring
Can I reuse a lancet?
It's better to use a single-use lancet each time. Reusing lancets can make finger sticks more uncomfortable and less clean.
Should I clean my finger with alcohol?
Soap and warm water is usually the better choice for routine home testing. Dry your hands well before testing.
What if I don't get enough blood on the strip?
Warm your hands, lower your hand briefly, and try again with better blood flow. Don't squeeze the finger aggressively.
Do I need to keep a log if my meter stores results?
Yes. The number alone isn't enough. Add context such as fasting, after-meal, exercise, symptoms, and medication timing.
Is a CGM always better than a glucometer?
No. A CGM gives trend data, but some people do very well with a standard meter. The better device is the one that matches your treatment plan and the routine you can sustain.
What if I keep putting off testing?
That's common. Pain, anxiety, frustration, and burnout can all get in the way. If that keeps happening, tell your clinician directly so the plan can be adjusted.
If you need help building a realistic blood sugar monitoring plan, reviewing your readings, or choosing between a glucometer and a CGM, Maryland Primary and Urgent Care offers primary care follow-up for adults managing diabetes and other chronic conditions. Dr. Sherif Hassan and the team can help you turn home readings into a plan that fits your daily life.
