Urgent care is the right choice for non life-threatening problems that need prompt attention, such as minor cuts, sprains, fevers, and infections. It also helps keep emergency rooms available for true emergencies, with research showing a 17.2% decrease in total emergency department visits in ZIP codes with an open urgent care center, driven mainly by a 27% reduction in nonurgent visits.
If you’re deciding what to do right now, the question usually isn’t just “urgent care or ER.” It’s which setting fits your symptoms, how fast you need help, and whether you need hands-on testing, treatment, or immediate emergency support. That’s where a simple four-way framework helps.
Table of Contents
- Do I Need the ER or Can It Wait? An Introduction
- Understanding Your Four Main Care Options
- Care Comparison Chart Conditions Costs and Wait Times
- Red Flag Symptoms Go Straight to the ER
- What to Expect at Maryland Primary and Urgent Care
- A Quick Checklist for Your Care Decision
- Frequently Asked Questions About Urgent Care
Do I Need the ER or Can It Wait? An Introduction
A common situation goes like this. It’s after work, your ankle is swelling after a misstep, your child has a fever, or you’ve had a sore throat that suddenly got worse. You know you need care, but you don’t know whether it’s serious enough for the ER, simple enough to wait for your doctor, or something urgent care should handle.
Urgent care sits in the middle. It’s for medical issues that need same-day attention but aren’t severe enough for an emergency room. That includes many minor injuries and acute illnesses that feel too important to ignore, but don’t come with signs of immediate danger.
For many patients, the safest first question is this: Is this life-threatening or quickly getting worse? If the answer is yes, go to the ER. If the answer is no, the next step is deciding whether you need in-person care today, a scheduled primary care visit, or a telemedicine appointment.
If you want a focused breakdown of that first decision, this guide to urgent care vs ER choices is useful for sorting out where immediate treatment belongs.
Practical rule: If the problem is painful, new, and needs attention today, urgent care is often the right lane. If the problem threatens breathing, circulation, brain function, or severe internal injury, it isn’t.
That distinction matters because people often judge urgency by discomfort alone. Pain matters, but severity is not the same as danger. A high fever, minor laceration, sprain, or sinus infection may feel miserable and still fit urgent care. Chest pain, stroke symptoms, severe shortness of breath, or major trauma do not.
Understanding Your Four Main Care Options

Often, the decision comes down to two choices: urgent care or ER. In practice, you have four main options. Knowing the role of each one makes the decision much easier when symptoms start suddenly.
A good overview of the difference between urgent care and primary care helps, but the short version is that each setting answers a different kind of medical need.
Primary care handles the planned and the familiar
Primary care is best for routine care, chronic disease management, follow-up, preventive visits, medication review, and non-urgent symptoms that can wait for an appointment. Your primary care clinician knows your history, medications, allergies, and baseline health.
That context matters when the issue is not time sensitive. Ongoing blood pressure management, diabetes follow-up, recurring headaches, preventive screening, travel planning, and medication adjustments usually fit here better than urgent care.
Urgent care fills the gap
Urgent care is built for same-day problems that need evaluation and treatment but are not life-threatening. The technical distinction matters. According to Blue Cross Blue Shield guidance on primary care, urgent care, and emergency room use, urgent care appropriately manages sprains, strains, minor lacerations, fever, and acute infections, meaning conditions with rapid onset but stable vital signs.
That “stable vital signs” piece is what patients often miss. A condition can be uncomfortable, disruptive, or painful and still be medically stable enough for urgent care. Examples include:
- Infections: sore throat, ear pain, sinus symptoms, urinary symptoms
- Minor injuries: ankle sprains, minor burns, small cuts that may need closure
- Acute but contained symptoms: fever, rash, mild dehydration, medication side effects without severe reaction
Urgent care works best when you need prompt in-person care, but you don’t need hospital-level emergency resources.
ER care is for unstable or potentially life-threatening symptoms
Emergency departments are for conditions where delay could put life, limb, or organ function at risk. The same BCBS guidance states that severe chest pain, difficulty breathing, or stroke symptoms mandate emergency department evaluation.
The ER is also the right place when you may need intensive monitoring, advanced imaging, emergency procedures, or admission to the hospital.
Telemedicine works best when a physical exam is not the main need
Telemedicine is useful when the main need is advice, symptom review, medication discussion, straightforward follow-up, or an initial assessment. It’s convenient, fast, and often the easiest step if you’re not sure whether you need to be seen in person.
It’s less useful when the clinician needs to listen to your lungs, examine an injury, test urine, perform a swab, close a wound, or rule out a more serious physical finding. In those cases, telemedicine can guide you, but it usually won’t finish the job.
Care Comparison Chart Conditions Costs and Wait Times
The most practical way to decide when to visit urgent care is to compare it directly with your other options. Urgent care centers don’t just offer convenience. They also change how communities use emergency services. In this study on urgent care expansion and emergency department use, researchers found a 17.2% decrease in total ED visits for residents in ZIP codes with an open urgent care center, mainly from a 27% reduction in nonurgent visits. The drop was even greater among uninsured patients at 21% and Medicaid patients at 29.1%.
That finding supports a practical point patients see every day. Choosing the right setting is not just about saving time. It improves access for everyone and keeps the ER focused on emergencies.
Choosing the right care by symptom and timing
| Condition / Factor | Primary Care Physician (PCP) | Urgent Care Center | Emergency Room (ER) | Telemedicine |
|---|---|---|---|---|
| Cold, flu, sore throat | Good if you can get a prompt appointment and symptoms are mild to moderate | Strong choice if symptoms need same-day testing or treatment | Not appropriate unless severe breathing trouble or other red flags are present | Good first step for symptom review and guidance |
| Fever without emergency signs | Appropriate during office hours | Good if fever needs same-day evaluation | ER only if fever comes with severe danger signs | Useful for early advice if the patient looks stable |
| Minor cut or laceration | Sometimes, if same-day wound care is available | Often the best fit for cleaning, closure, and dressing | ER if bleeding is severe or the wound is deep and complicated | Not suitable if the wound needs hands-on care |
| Sprain or strain | Good for follow-up | Good for prompt assessment and support care | ER if deformity, severe trauma, or major loss of function is present | Limited. Helpful only for initial guidance |
| Possible minor fracture | Usually not the first choice for immediate care | Often appropriate if imaging is available on site | ER if injury is severe, limb is cold or numb, or pain is extreme | Not enough by itself |
| Chest pain | Not appropriate for new severe symptoms | Not appropriate if serious cause is possible | Correct setting | Not appropriate |
| Stroke-like symptoms | Not appropriate | Not appropriate | Correct setting immediately | Not appropriate |
| Medication refill or chronic issue review | Best setting | Sometimes, but not ideal for ongoing management | Not appropriate | Often a good option |
| Rash or pink eye | Good | Good if you need same-day treatment | ER only if part of a severe reaction or major illness | Often a good option |
| Relative cost | Usually lowest for planned care | Lower than ER for appropriate conditions | Highest for non-life-threatening issues | Often lower for simple visits |
| Wait pattern | Depends on schedule availability | Built for walk-ins and same-day needs | Variable, often longest for noncritical problems | Often convenient if the issue can be handled remotely |
For clinic operators, referral networks, and practices thinking about access strategy, the mechanics behind this matter. Work on getting more Catskill urgent care patients highlights how urgent care demand often grows when patients are given clearer symptom-based guidance rather than broad marketing promises.
What the chart means in real life
Three trade-offs decide most cases:
- Speed matters most: Choose urgent care when you need care today and the problem is stable.
- Continuity matters most: Choose primary care when the issue is ongoing, preventive, or tied to long-term management.
- Risk matters most: Choose the ER when a bad outcome could happen if you wait.
If your question is “Can this wait until tomorrow?” and the answer is “probably not, but I’m not in danger,” that’s the classic urgent care decision.
Red Flag Symptoms Go Straight to the ER

Some symptoms are not urgent care problems. They are emergency problems. When these show up, the right move is immediate ER evaluation or calling 911.
Symptoms that should not wait
- Severe chest pain: Especially if it feels crushing, heavy, or comes with sweating, nausea, faintness, or shortness of breath
- Difficulty breathing: Breathing that is labored, worsening, or associated with blue lips, confusion, or inability to speak normally
- Stroke symptoms: Sudden facial droop, arm weakness, numbness, trouble speaking, confusion, or sudden vision changes
- Severe abdominal pain: Intense pain, rigid abdomen, repeated vomiting, or pain with fainting or major weakness
- Major trauma: Serious car accident injuries, major falls, deep wounds, heavy bleeding, or obvious deformity
- Loss of consciousness or seizure
- Severe allergic reaction: Swelling of the face or throat, trouble breathing, or rapid worsening after exposure
- Severe bleeding: Bleeding that doesn’t stop with pressure
These are the situations where delay can be dangerous. Urgent care isn’t designed for hospital-level emergency response.
A short visual review can help reinforce the decision points:
When uncertainty should still push you to emergency care
Sometimes the symptom list doesn’t feel perfectly clear, but the patient clearly looks very unwell. Trust that signal.
Go to the ER if symptoms are rapidly worsening, the person seems confused or hard to wake, or something feels seriously wrong in a way that can’t be monitored safely at home.
What doesn’t work is trying to “wait and see” when the problem involves breathing, neurological change, severe pain with collapse, or uncontrolled bleeding. In those cases, choosing the ER early is safer than trying urgent care first.
What to Expect at Maryland Primary and Urgent Care
For many patients, the most useful part of urgent care is simple: it removes the friction between “I need help today” and “I can’t get into my regular doctor.” The visit is usually straightforward, and knowing what to expect makes the decision easier.
When timing can make your visit easier
Timing changes the experience. According to this urgent care timing guide, emergency department use rises on weekends, including a 17.8% increase on Saturdays, while 92% of urgent care centers report waits under 30 minutes, with most visits completed in under an hour. The same source notes that visiting on a weekday morning is often the best strategy for the shortest wait.
That matches what works operationally in busy community medicine. If your issue is stable, early mornings and weekdays are usually easier than after-work surges and weekend peaks.
If you want a practical overview of services and access, the advantages of a Maryland primary care and urgent care clinic show how combined care settings can help patients move from urgent treatment to follow-up without starting over elsewhere.
What a typical urgent care visit looks like
A usual urgent care visit has four parts:
Check-in
Bring your photo ID, insurance card if you have one, and a medication list. If you don’t have a written list, bring the bottles or a phone note with names and doses.Triage
Staff will ask why you’re there, check vital signs, and decide how quickly you need to be seen. This assessment helps distinguish urgent care from ER medicine. A stable patient with a painful but limited problem can usually stay in the urgent care lane.Evaluation and testing
Depending on symptoms, your visit may include an exam, point-of-care testing, lab work, or other office-based diagnostics. In a setting like Maryland Primary and Urgent Care, patients may also have access to on-site lab services and echocardiography, which can make same-day assessment more efficient for selected issues.Treatment and follow-up
You may leave with prescriptions, wound care instructions, activity guidance, or advice about when to return. Some patients need a primary care follow-up. Others need referral for specialist care. A small number need escalation to the ER based on what the clinician finds during the visit.
What doesn’t help is arriving without key information. If you can, bring:
- Identification: Photo ID and insurance card
- Medication details: Current medicines, doses, allergies
- Relevant records: Recent test results or discharge papers if this is a follow-up issue
- Timeline: When symptoms started and what changed
A Quick Checklist for Your Care Decision
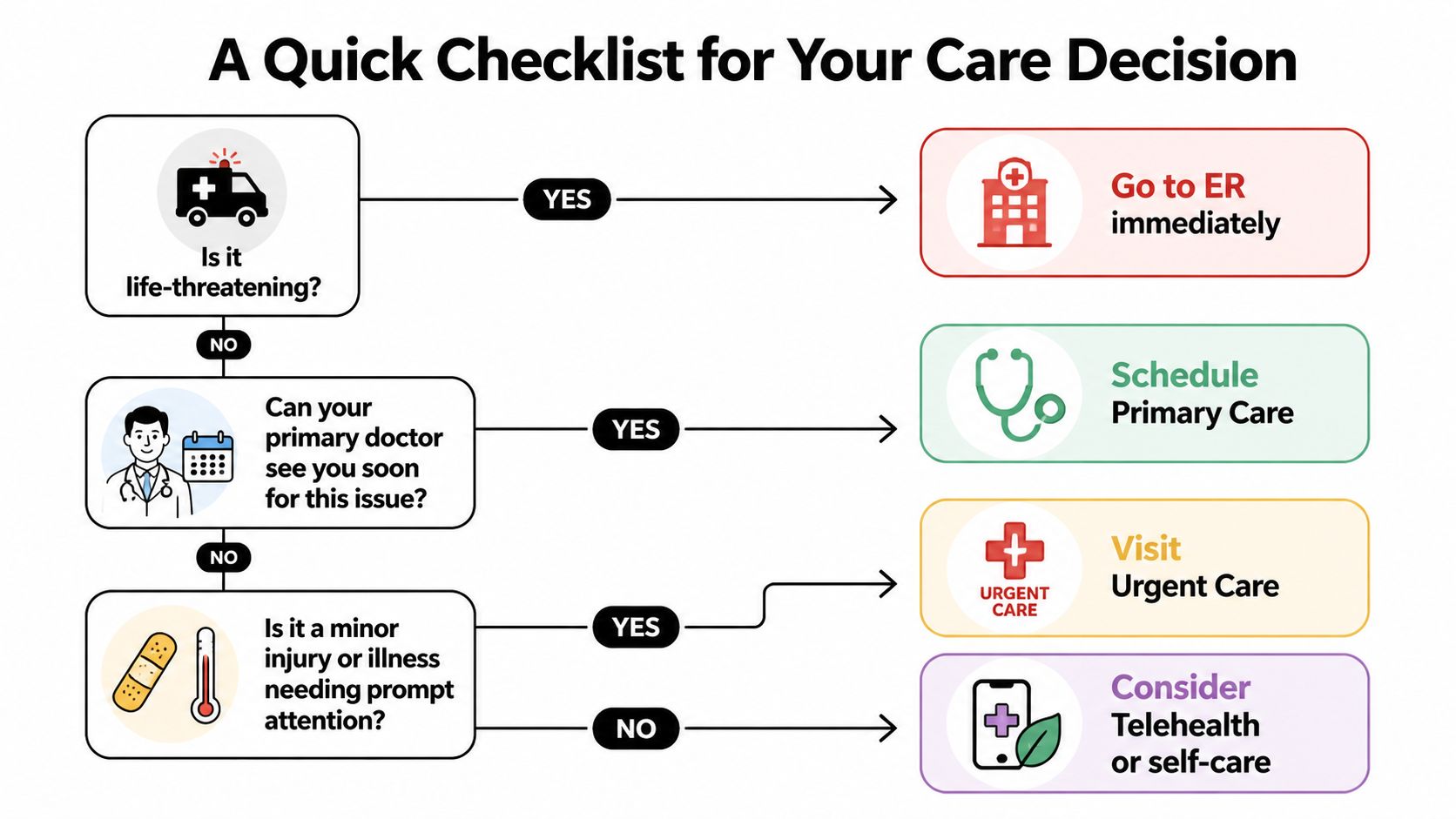
When symptoms start, you don’t need a long analysis. You need a short sequence of decisions that keeps you safe and gets you to the right place.
Use these four questions in order
Is it life-threatening?
If there is severe chest pain, difficulty breathing, stroke symptoms, severe bleeding, loss of consciousness, or major trauma, go to the ER immediately.If not, does it need same-day attention?
If the issue can safely wait a few days, schedule primary care. That’s often best for chronic concerns, medication review, preventive care, and symptoms that are bothersome but stable.Can it be handled remotely?
If the issue mainly needs advice, symptom review, or a simple follow-up discussion, telemedicine may be enough. If someone needs a physical exam, testing, wound care, or imaging, remote care usually won’t solve the whole problem.If it needs prompt in-person care and isn’t an emergency, choose urgent care.
This is the right answer for many fevers, sore throats, urinary symptoms, sprains, minor cuts, rashes, and infections.
The safest shortcut is this: emergency symptoms go to the ER, routine problems go to primary care, remote-friendly questions go to telemedicine, and stable same-day problems go to urgent care.
If you’re still unsure, call a medical office and describe the symptoms clearly. State what changed, how long it’s been going on, and whether the patient is getting worse. Good triage starts with a good description.
Frequently Asked Questions About Urgent Care
Do I need an appointment for urgent care?
Usually, no. Urgent care is designed for walk-ins and same-day needs. Some clinics also offer online booking, which can make the process smoother.
What should I bring to urgent care?
Bring a photo ID, your insurance card if you have one, a list of medications, and any recent records related to the problem. If the visit involves an injury, it also helps to know exactly when and how it happened.
Will urgent care handle follow-up care?
Urgent care usually handles the immediate problem first. If you need ongoing monitoring, repeat medication management, or specialist evaluation, the clinician may direct you back to your primary care doctor or refer you for additional care.
Is telemedicine enough for urgent problems?
Sometimes, but not always. Telemedicine works well for discussions, guidance, and some uncomplicated issues. It doesn’t replace hands-on exams, wound care, imaging, or most office testing.
When should I skip urgent care entirely?
Skip urgent care if symptoms suggest a true emergency. Severe chest pain, trouble breathing, stroke signs, severe bleeding, loss of consciousness, and major trauma belong in the ER.
Can urgent care help with chronic conditions?
It can help when a chronic condition has a new flare or acute change, but it’s usually not the best place for long-term management. Ongoing care still belongs with primary care.
If you need adult primary care, walk-in urgent care, same-day visits, telemedicine, lab services, travel care, or coordinated follow-up in Lanham and the surrounding region, Maryland Primary and Urgent Care offers practical, timely care built around what patients need most: clear guidance, efficient visits, and continuity after the immediate problem is addressed.
