Preventive health screenings for adults are age- and risk-appropriate medical tests that help find disease early, often before symptoms appear. Only 5.3% of adults age 35 and older received all recommended high-priority preventive services in 2020, far below the Healthy People 2030 target of 11.5%, which is why having a clear screening plan matters so much for long-term health (CDC data brief).
Preventive screening isn't a single test. It's a schedule of checks that changes as you age, your family history becomes clearer, and your risks shift. Following those recommendations is one of the most effective ways to protect lifespan and quality of life because many serious conditions are easier to manage when they are found early.
In day-to-day primary care, the biggest problem usually isn't that people reject prevention. It's that life gets in the way. Work, childcare, transportation, language barriers, fear of results, and not knowing which test matters now all lead to missed care. In a diverse community like Lanham, that practical gap matters just as much as the guideline itself.
Routine preventive care could save 100,000 lives annually in the United States, yet important screenings fell after the pandemic, including a 22% relative drop in colorectal cancer screening among Black adults and a 17% drop in breast cancer screening among Hispanic adults in 2021 (CDC data brief). That is the right frame for this topic. Preventive health screenings for adults aren't just a checklist. They're a way to close real care gaps before they become harder, more invasive, and more disruptive to treat.
Some screening visits also uncover issues patients didn't realize were connected, such as food-related symptoms, fatigue, or skin problems. If unexplained reactions are part of your picture, a careful symptom-based workup matters, and resources such as How to Test for Histamine Intolerance can help you understand what questions to bring to a clinician. If you're due for a broader preventive visit, an annual physical exam in Maryland primary care is often the simplest place to start.
Table of Contents
- Your Guide to Preventive Health Screenings
- Why Proactive Health Screenings Matter
- Essential Screenings for Young Adults Ages 18-39
- Key Screenings for Mid-Life Adults Ages 40-64
- Health Screenings for Older Adults Ages 65+
- How to Easily Access Your Screenings
- Frequently Asked Questions About Screenings
Your Guide to Preventive Health Screenings
Preventive health screenings for adults are tests, measurements, and conversations used to detect risk early. Some are simple vital sign checks. Some are blood tests. Others are cancer screenings or infection screening based on age, sex, family history, or personal risk.
The key point is that screening happens before you feel sick. That is different from diagnostic testing, which starts after symptoms appear. A cholesterol panel done to establish baseline risk is preventive. A scan ordered because you have chest pain is diagnostic.
In primary care, the most useful approach is simple:
- Start with your age group. This creates the default list.
- Add personal risk factors. Family history, smoking history, weight, blood pressure, sexual health history, and prior test results matter.
- Keep one home base for records. Scattered care leads to missed follow-up.
- Repeat tests at the right interval. More testing isn't always better.
Practical rule: The best screening plan is the one you can actually complete and repeat on time.
People often assume preventive care means a long, expensive process. Usually it doesn't. A standard preventive visit can organize what you need now, what can wait, and what should be tracked over time. That matters because many adults are either under-screened in high-risk areas or over-tested in low-risk ones.
A good screening plan should do three things well:
- Find silent problems early such as high blood pressure, lipid disorders, or diabetes risk.
- Match testing to real risk instead of using a one-size-fits-all checklist.
- Reduce friction so you don't need multiple appointments for basic care.
For adults in Lanham and Prince George's County, practical access matters just as much as medical advice. Walk-ins, same-day visits, on-site labs, and clear follow-up can make the difference between intending to get screened and getting it done.
Why Proactive Health Screenings Matter
Waiting for symptoms sounds reasonable until you remember how many serious conditions stay quiet for years. High blood pressure, high cholesterol, diabetes, cervical cell changes, and some early cancers often don't announce themselves. By the time symptoms show up, the problem may already be more advanced.
That is why preventive care works like maintenance on a car. You don't check the brakes because the car has already crashed. You check them so the crash doesn't happen.

What screening changes
A preventive test usually does one of three jobs:
- It finds a hidden condition such as high blood pressure or abnormal cholesterol.
- It establishes a baseline so future changes are easier to interpret.
- It identifies who needs closer follow-up and who doesn't.
That middle point gets overlooked. A baseline matters because medicine is rarely one lab value in isolation. A clinician wants to know whether something is new, stable, worsening, or responding to treatment.
Dental prevention offers a useful comparison. People don't usually wait for a severe toothache before improving daily habits. The same idea applies to whole-body health, and practical prevention habits matter in multiple areas of care. For readers thinking about day-to-day prevention beyond the medical office, this guide on how to prevent cavities is a good example of how small routine actions can prevent larger problems later.
Prevention is more than testing
Screenings are only part of preventive medicine. The visit itself often includes discussion of sleep, weight change, tobacco use, alcohol use, exercise, stress, sexual health, and medications. Those details influence what should be screened and how often.
A screening schedule should fit your actual life. Night-shift work, caregiving, recent immigration, and transportation problems all affect whether a plan is realistic.
For example, a patient with a strong family history of heart disease may need earlier and more frequent attention to cardiovascular risk. A patient with no smoking history does not need the same lung cancer screening pathway as someone with substantial tobacco exposure. That kind of precision is the difference between useful prevention and random testing.
If you're concerned specifically about cardiovascular risk, this overview of why early cardiovascular screening is crucial for your health explains why waiting for symptoms can be a costly mistake.
Essential Screenings for Young Adults Ages 18-39
Young adulthood is when many people feel healthy enough to skip care. That's exactly why this age group benefits from screening. The goal isn't to search for disease everywhere. It's to establish baselines, catch silent risk early, and identify habits or exposures that can change long-term health.

The baseline tests that matter early
For most adults in this age range, the foundation includes blood pressure checks, weight and metabolic risk review, mental health screening during primary care, and age-appropriate sexual health screening based on exposure and history. Cervical cancer screening also begins in adulthood and follows a defined interval schedule.
Cholesterol deserves special attention. High low-density lipoprotein, or LDL, approximately doubles heart-attack risk, and the USPSTF recommends cholesterol screening beginning at age 20 to establish a cardiovascular baseline. A reduction of 39 mg/dL in LDL can decrease major vascular events by about 20% (preventive screening guide).
That does not mean every young adult needs medication. It means every young adult benefits from knowing where they stand.
What to ask for at this age
A practical young-adult screening visit often includes:
- Blood pressure review to identify early hypertension or rising trends.
- Lipid panel to establish cardiovascular baseline and guide future follow-up.
- Weight and metabolic risk discussion especially if there is overweight, obesity, family history, or prior abnormal labs.
- Cervical screening when applicable based on age and prior results.
- STI screening based on sexual history rather than assumptions.
- Mental health screening because anxiety, depression, sleep disruption, and stress often surface early in adult life.
Common mistakes in this age group
The most common problem is not a lack of recommendations. It's delayed follow-through. Young adults often come in only for urgent issues, job forms, or school requirements. That can miss quiet problems that are much easier to address now than later.
Another mistake is assuming fitness cancels risk. An active person can still have high cholesterol. A person at a healthy weight can still have depression, cervical screening needs, or sexually transmitted infection risk. Prevention works best when it is based on actual risk, not appearance.
If you're in your twenties or thirties, the goal is not to do everything. The goal is to get the right baseline and build a habit of periodic review.
For immigrant patients, young adulthood is also a period when preventive care may be fragmented. Someone may have completed school forms, immigration exams, or urgent visits without building an ongoing primary care relationship. In that situation, a dedicated preventive visit is often the first chance to organize vaccines, lab work, and screening history into one plan.
Key Screenings for Mid-Life Adults Ages 40-64
Mid-life is where preventive care usually becomes more concrete. Risks for diabetes, cardiovascular disease, and several cancers rise. This is also the age range where screening decisions start to feel more personal because family history, smoking history, prior lab trends, menopause, and long-standing habits begin to shape the schedule.
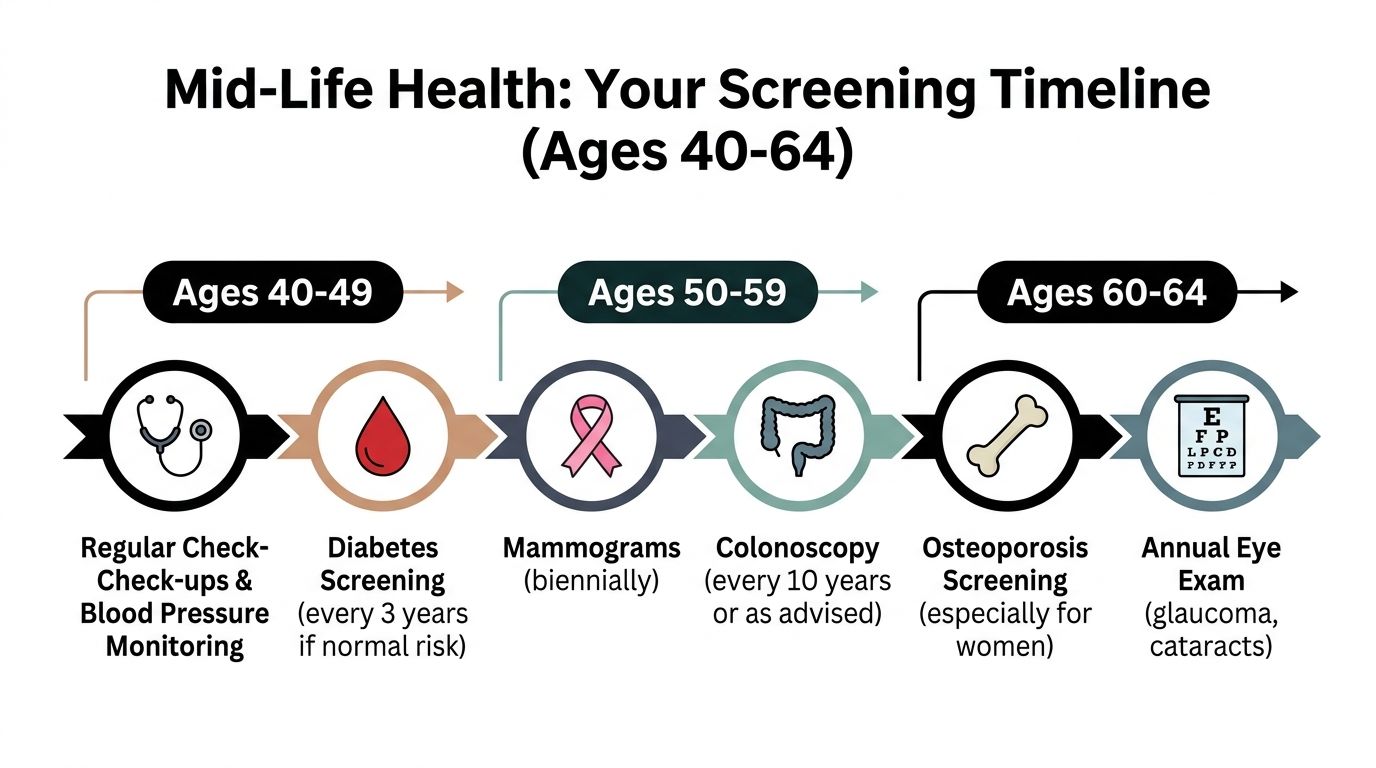
A practical screening table
| Screening Test | Ages 18-39 | Ages 40-64 | Ages 65+ |
|---|---|---|---|
| Blood pressure | Regular checks based on primary care guidance and risk | Ongoing monitoring becomes more important | Ongoing monitoring remains essential |
| Cholesterol or lipid panel | Baseline screening begins in adulthood | Repeat based on prior results and cardiovascular risk | Continue based on health status and treatment goals |
| Diabetes screening | Consider based on risk, especially overweight or obesity | Commonly relevant in this age range | Continue based on overall health and prior history |
| Cervical cancer screening | Applies in adult years when relevant | Continue through eligible years at recommended intervals | May stop after guideline-based age and history review |
| Breast cancer screening | Usually not routine for most younger adults at average risk | Important in eligible age groups | Continue selectively through later eligible years |
| Colorectal cancer screening | Usually not routine for most younger adults at average risk | Becomes a major priority in mid-life | Continue through appropriate later ages |
| Lung cancer screening | Only for adults meeting smoking-related criteria | Important for eligible smokers or former smokers | Continue only if criteria still apply |
| Bone health and fall risk | Usually risk-based | Begins to matter more, especially for some women | Becomes a major focus |
A table like this is useful, but it can mislead if you read it as fixed rules. The details still matter. A patient with prior abnormal findings, strong family history, or tobacco exposure may need a different schedule than a same-age patient without those factors.
Why intervals are different
Screening intervals are not arbitrary. They are calibrated to how the disease behaves and who is most likely to benefit. Cervical cancer screening can extend from every 3 years to every 5 years for women over 30 using HPV testing, while lung cancer screening is reserved for adults age 50 to 80 with a significant smoking history (USPSTF recommendations).
That difference explains an important trade-off in preventive medicine. More testing is not automatically better. Over-screening can produce false alarms, extra procedures, anxiety, and cost. Under-screening misses the period when disease is easiest to treat.
What most adults need to discuss in mid-life
For many patients between 40 and 64, these are the high-value conversations:
- Diabetes screening if weight, blood pressure, family history, or prior labs raise concern.
- Breast cancer screening based on age and personal risk.
- Colorectal cancer screening once age and eligibility criteria are met.
- Lung cancer screening only if smoking history fits the criteria.
- Prostate screening discussion as a shared decision rather than an automatic test.
- Ongoing cholesterol and blood pressure review because cardiovascular risk often accelerates in this period.
Mid-life also reveals practical barriers. A parent caring for children and older relatives may delay colon cancer screening because prep and scheduling feel disruptive. A self-employed adult may postpone follow-up because time off work is hard to arrange. Those are not small issues. They are often the main reason care gets delayed.
The right screening recommendation can still fail if the logistics are unrealistic. Access, timing, and follow-up are part of good medicine, not extras.
Health Screenings for Older Adults Ages 65+
After 65, preventive care shifts from early detection alone to preserving independence, mobility, and daily function. Cancer screening still matters for some adults, but other priorities move higher on the list. Bone health, fall risk, medication review, vision, hearing, memory concerns, and blood pressure control can affect quality of life as much as any lab result.
What becomes more important after 65
Many older adults benefit from focusing on the conditions that most often change day-to-day safety and function:
- Bone health review because fractures can dramatically reduce mobility and independence.
- Vision and hearing checks when changes start affecting driving, communication, or falls.
- Medication review to identify duplication, side effects, or interactions.
- Fall risk assessment especially after imbalance, weakness, or a near fall.
- Cognitive and mood review when memory changes, confusion, or withdrawal from activities appears.
These aren't minor concerns. They determine whether someone can live confidently at home, manage medications correctly, and stay active.
When it may make sense to stop a screening
Not every screening should continue forever. In later life, good preventive care becomes more individualized. The question shifts from "Is this test recommended at my age?" to "Will this test help me live better or longer, given my health status and goals?"
That is why shared decision-making matters more in this age group. Some adults remain healthy and active and continue selected cancer screening. Others have enough medical complexity that the burden of testing outweighs the likely benefit.
Insurance and care coordination also become more important for older patients and their families. For caregivers trying to understand practical coverage questions, this guide on health insurance for elderly parents can be a useful planning resource alongside a primary care discussion.
A good older-adult preventive visit should leave you with a simple answer to three questions: what needs attention now, what can safely wait, and what no longer adds value.
How to Easily Access Your Screenings
About half of U.S. adults delay or skip recommended health screenings, often because the process feels hard to fit into daily life, according to Fierce Healthcare's coverage of national survey findings. In Lanham, I see the same pattern in clinic every week. The issue is rarely a lack of concern about health. It is the gap between what national guidelines recommend and what a person can realistically complete while managing work, childcare, transportation, language barriers, or insurance questions.
A good screening plan has to work in real life. The best screening plan is the one you can complete.
For many adults, the sticking point is not the test itself. It is the number of steps. One visit for the annual exam, another for blood work, time off for imaging, then a separate follow-up call. Each extra step raises the chance that screening gets postponed.
In Lanham, that burden can be heavier for immigrants, recent arrivals, and patients without a regular primary care office. Some have completed urgent visits or immigration-related medical exams but have never had a clinician review what preventive care is due by age, sex, family history, and risk factors. Others are unsure which services are covered as preventive, what requires a copay, or where to go if they need help in a language they understand.
What makes access easier is straightforward coordination:
- One primary care visit to sort out priorities
- Lab testing available in the same setting
- Clear instructions on what is due now and what can wait
- Telemedicine for follow-up when an office visit is not needed
- Walk-in or same-day options when schedules are tight
That is one reason local clinics matter. Maryland Primary and Urgent Care provides adult primary care, walk-ins, same-day appointments, telemedicine in several states, USCIS civil surgeon exams, and on-site lab services for common screening tests. For patients with transportation limits or unpredictable work hours, reducing extra stops can make the difference between planning screening and finishing it.
If you are overdue, start small and be specific:
- Book one preventive visit. Let the clinician build the list with you instead of trying to piece it together on your own.
- Bring any records you have. A portal screenshot or photo of past results is often enough to avoid repeating tests.
- Write down your family history before the visit. Include who had the condition and about what age it started.
- Ask for a prioritized plan. Some tests are due now. Others can wait a few months.
- Clarify cost before you leave. Ask which items are preventive and which could become diagnostic if symptoms are involved.
This matters even more for patients who are new to the U.S. health system. Preventive care here is often spread across visits, referrals, labs, and insurance rules that are not obvious at first. A clinic that handles both immediate needs and routine primary care can help close that gap and give patients one place to return with questions.
A short explainer can also help if you haven't booked preventive care in a while:
Good preventive care should feel organized, not overwhelming. For many adults in Lanham, the first useful step is simple. Choose a regular clinic and ask, "What am I due for right now?"
Frequently Asked Questions About Screenings
Does family history change when I should be screened
Yes. Family history can change both the starting age and the intensity of screening. If a parent, sibling, or child had certain cancers, early heart disease, diabetes, or lipid disorders, tell your clinician clearly and early. The details matter, including which relative, what condition, and roughly what age it appeared.
Is genetic testing the same as preventive screening
No. Genetic testing and preventive screening overlap in some cases, but they are not the same thing. Screening usually looks for early disease or risk markers in the general population or in people with defined risk. Genetic testing is more selective and is typically considered when personal or family history suggests an inherited condition.
What if one of my screening results is abnormal
An abnormal result does not always mean you have a serious disease. It usually means you need context. Some results need repeat testing. Others need imaging, a procedure, or a referral. The most important next step is prompt follow-up with the clinician who ordered the test so the result is interpreted in light of your symptoms, history, medications, and prior values.
Are immigration medical exams the same as routine preventive care
No. Immigration exams serve a specific legal purpose. They may include vaccinations and required testing, but they do not replace complete preventive care. If you've completed an immigration exam, you may still need age-appropriate screenings, chronic disease review, and routine follow-up through primary care.
How often should I get screened if I feel fine
That depends on age, sex, personal risk, prior results, and family history. Feeling fine doesn't rule out silent conditions such as high blood pressure or abnormal cholesterol. The safest approach is to review your preventive schedule with a primary care clinician and set reminders for the next due dates.
If you're ready to stop guessing about what tests you need, Maryland Primary and Urgent Care can help you sort out which screenings are appropriate now, which can wait, and how to complete them with as few barriers as possible. A clear preventive plan is easier to follow when your visit, lab work, and follow-up are coordinated in one place.
