Yes, allergies are a common cause of sore throats, and postnasal drip is the main reason. In allergy-related cases, specialists identify postnasal drip as the primary mechanism in up to 80% of cases, and in the U.S. seasonal allergic rhinitis affects about 60 million people annually, with sore throat reported in 30 to 40% of cases during peak pollen seasons.
If you woke up with a scratchy throat, feel irritated rather than sick, and keep noticing sneezing, clear drainage, or itchy eyes, allergies may be the problem. That's especially relevant in Lanham and across Prince George's County, where seasonal pollen and other airborne triggers can make a sore throat linger long after a cold would usually pass.
Table of Contents
- Yes Allergies Are a Common Cause of Sore Throats
- The Science Behind an Allergy Sore Throat
- Is It Allergies a Cold or Strep Throat
- At-Home and Over-the-Counter Relief
- When to See a Doctor for Your Sore Throat
- Frequently Asked Questions about Allergy Sore Throats
Yes Allergies Are a Common Cause of Sore Throats
A lot of people assume a sore throat always means infection. That's not true. Allergies are a leading cause of sore throats, and seasonal allergic rhinitis affects approximately 60 million people in the U.S. annually. During peak pollen seasons, 30 to 40% of those cases include sore throat as a symptom, according to CDC and AAAAI data summarized here.
What makes allergy throat pain easy to miss is that it often feels mild at first. People describe it as scratchy, dry, irritated, or annoying rather than sharply painful. They may still go to work, run errands, and function normally, which makes them think it can't be significant.
What this usually feels like
Common patterns include:
- Morning irritation: Your throat feels worse when you wake up because mucus has been draining overnight.
- Clear allergy symptoms: Sneezing, nasal congestion, and itchy eyes show up along with throat discomfort.
- No fever: You feel bothered, not severely ill.
- Longer course: The throat stays irritated as long as exposure continues.
Practical rule: If your throat keeps hurting during pollen exposure but you don't have fever or a sudden severe illness, allergies belong high on the list.
Indoor air can also keep symptoms going. Dust, pet dander, and circulating irritants often matter more than people realize. For patients trying to reduce household triggers, practical environmental changes can help, including the health benefits of duct cleaning for allergies when dust buildup and airflow issues are part of the problem.
The Science Behind an Allergy Sore Throat
An allergy sore throat usually starts in the nose, not the throat. The throat becomes the downstream victim.
When allergens enter the airway, they trigger mast cells to release histamine. That sets off a chain reaction. Histamine increases mucus production and contributes to swelling in the nasal passages and throat tissues. The extra mucus then drains down the back of the throat and irritates the pharyngeal lining. That's why allergy-related sore throats often come with clear, watery nasal discharge and no fever, as described in this clinical explanation of histamine and postnasal drip.
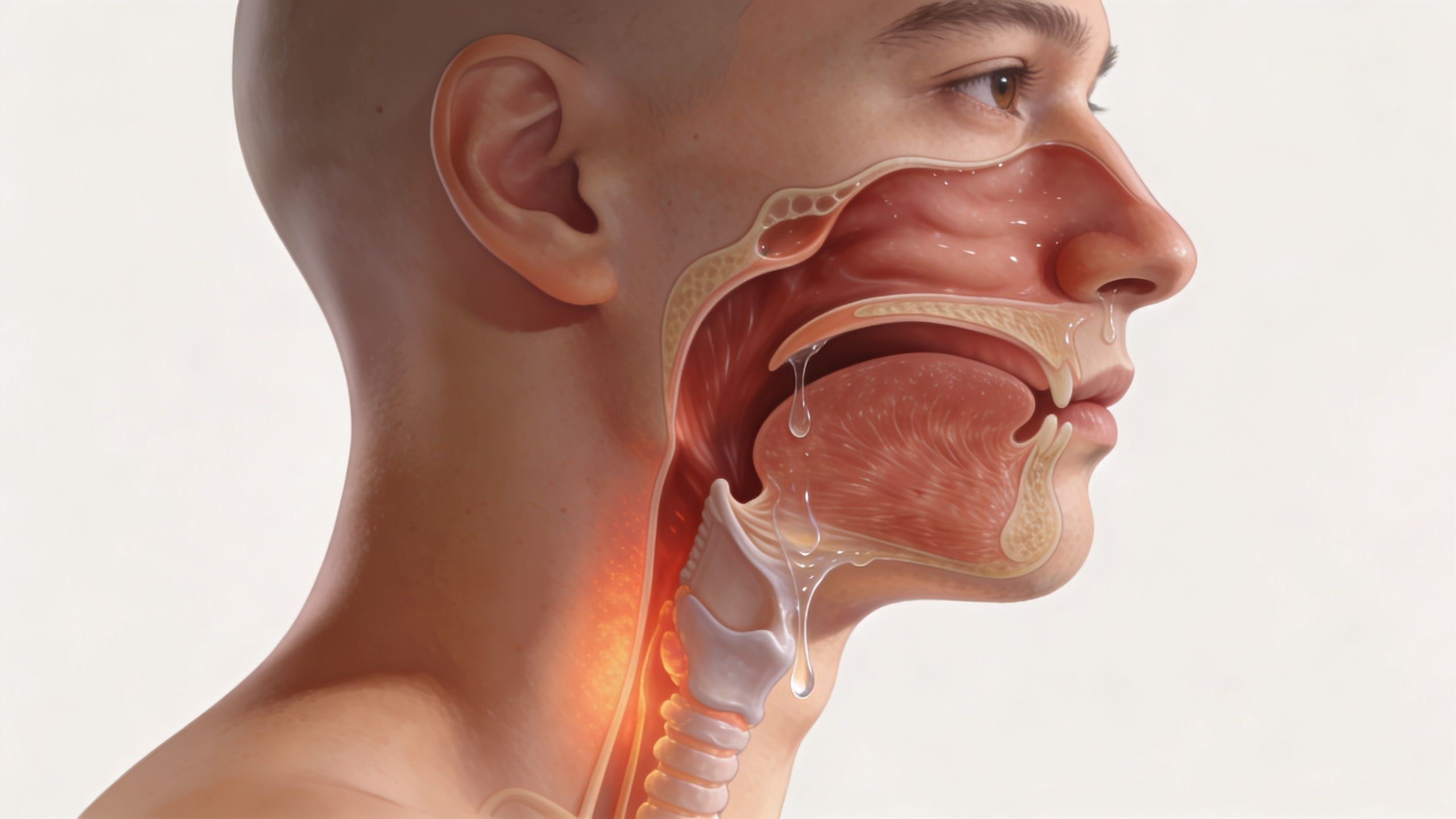
Think of it like a slow leaky faucet
A useful way to picture postnasal drip is a faucet that never fully turns off. The drip isn't dramatic, but it's constant. Over hours and days, that repeated contact makes the throat feel raw, scratchy, and inflamed.
The throat also gets irritated by behaviors that allergies trigger:
- Mouth breathing: A blocked nose makes you sleep with your mouth open, which dries throat tissues.
- Frequent throat clearing: Repeated clearing adds friction to already irritated tissue.
- Coughing from drainage: Even a mild cough can keep the inflammation going.
Ongoing drainage causes more trouble than one intense episode. That's why allergy throat symptoms often feel stubborn rather than dramatic.
Why this matters for treatment
If postnasal drip is driving the problem, treatment needs to target the allergy process and the mucus itself. Antibiotics won't fix histamine release. Random cough drops may soothe briefly, but they won't stop the drainage.
When the diagnosis is uncertain, testing can help separate allergic symptoms from infectious illness. In some situations, clinicians also use more advanced diagnostics for infectious causes, such as PCR analyzing for illnesses of an infectious nature, when the symptom picture doesn't fit a simple allergy pattern.
Is It Allergies a Cold or Strep Throat
This is the question that matters most in real life. The treatment changes depending on the cause, and guessing wrong often leads to wasted time, unnecessary medication, or delayed care.
A sore throat from allergies usually builds alongside other allergy symptoms. Strep is different. It often feels abrupt and much more intense. A key differentiator is that strep often presents with sudden severe pain, fever over 100.4°F, and white patches on the tonsils, while allergy sore throats are typically itchy, persistent without fever, and accompanied by sneezing and itchy eyes, as outlined in this allergy versus strep comparison.
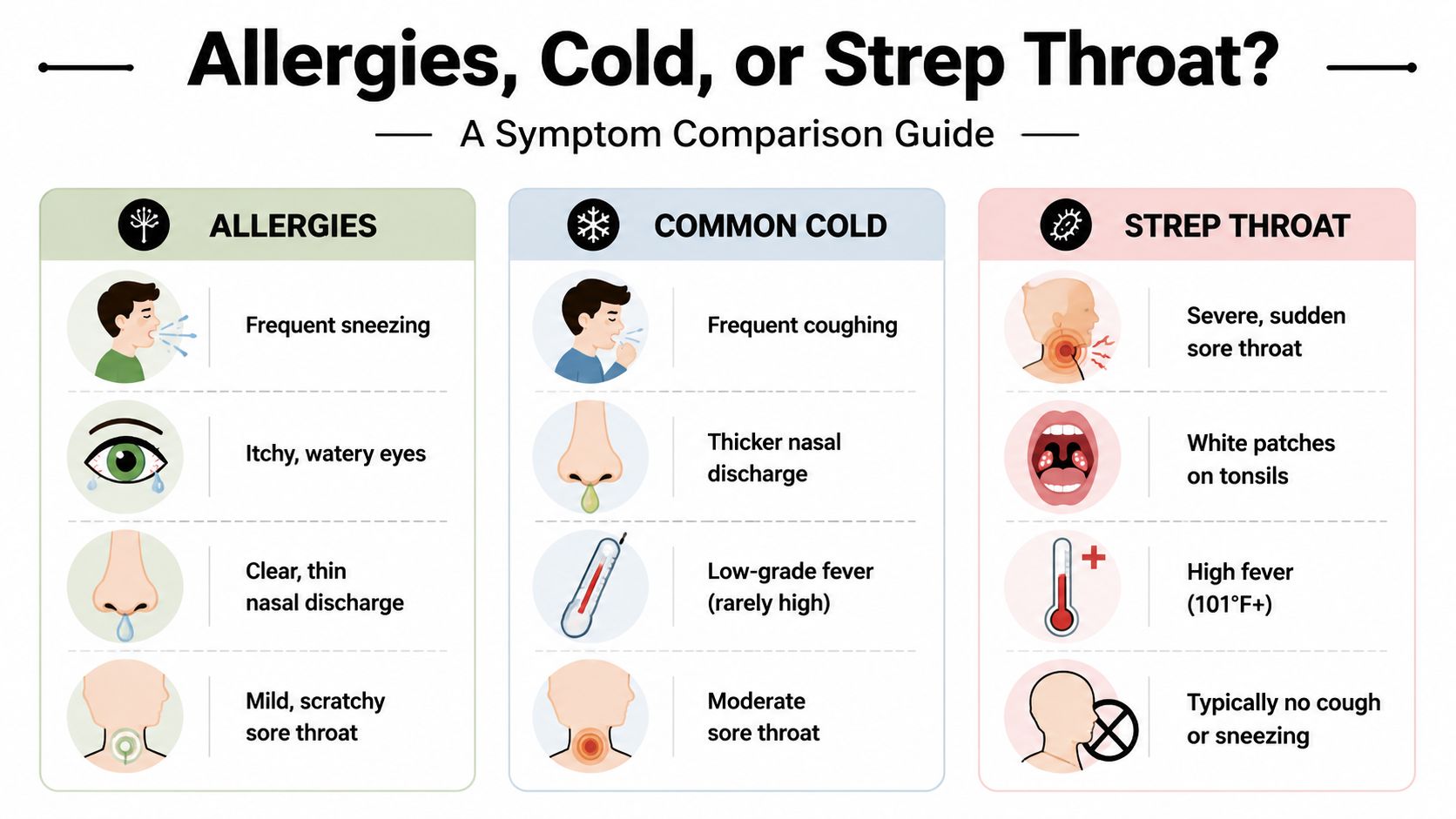
Symptom Checker table
| Symptom | Allergies | Cold (Viral) | Strep Throat (Bacterial) |
|---|---|---|---|
| Onset | Often gradual or tied to exposure | Usually gradual | Often sudden |
| Fever | Usually absent | Can occur | Common and more concerning |
| Nasal drainage | Clear and watery | Often thicker as illness progresses | Usually not the main feature |
| Itchy eyes or sneezing | Common | Less typical | Uncommon |
| Throat feeling | Itchy, scratchy, irritated | Sore with other cold symptoms | More severe pain |
| White tonsil patches | Not typical | Not typical | Can be present |
| Body aches | Less typical | More common than with allergies | Can occur |
| Cough | Can happen from drainage | Common | Often absent |
For some patients, food reactions add confusion. If throat symptoms seem tied to eating rather than pollen, dust, or pet exposure, it helps to understand the difference between allergy and non-allergic food reactions. This overview of food intolerance and allergy differences is a useful companion topic.
When the pattern points away from allergies
You should think beyond allergies if you have:
- Sudden severe throat pain: Especially if it becomes hard to swallow.
- Fever: This shifts the concern toward infection.
- White patches on the tonsils: A classic reason to test for strep.
- No sneezing or itchy eyes: That weakens the allergy case.
- A recent flu-like illness with lingering cough: Some patients continue coughing after a viral infection, and that can irritate the throat even after the worst symptoms fade. This is a different pattern than allergies and is explained in cough after flu.
For immigrants, asylum seekers, and patients with limited access to regular care, this distinction matters even more. Language barriers and delayed evaluation can make self-diagnosis harder. A sore throat that seems “probably allergies” can still be strep, COVID-19, reflux, or another condition that needs proper testing.
At-Home and Over-the-Counter Relief
The best relief comes from doing two things at once. First, calm the allergic reaction. Second, soothe the throat that's already irritated.

Simple home remedies
These don't cure allergies, but they often make the throat much more comfortable:
- Warm fluids: Tea with honey, broth, and warm water can reduce dryness and make swallowing easier.
- Saltwater gargles: This can soothe irritated tissue and help clear residual mucus from the throat.
- Hydration: Drinking enough water keeps secretions thinner and less sticky.
- Humidified air: If indoor air is dry, a humidifier can reduce irritation overnight.
- Shower and change clothes after being outdoors: This reduces pollen that would otherwise keep circulating around you.
If your throat is irritated from drainage, comfort measures work best when you also reduce the trigger. Soothing the throat without addressing the allergen only gives partial relief.
For indoor triggers, some patients also improve when they clean up the air they breathe at home, especially in bedrooms. If you're comparing options, these allergy purifiers from EcoQuest are one example of the type of environmental approach people consider alongside medication.
Effective over-the-counter options
Over-the-counter treatment works best when you choose the right tool for the symptom pattern:
- Antihistamines: These help block the histamine response driving sneezing, runny nose, and drainage.
- Saline nasal rinse or spray: This helps wash allergens and mucus out of the nasal passages.
- Nasal steroid sprays: These are often more useful for ongoing nasal inflammation than throat lozenges are.
- Lozenges: Good for temporary soothing, but limited if drainage is the main problem.
A common mistake is relying only on cough drops while ignoring the nose. Another is taking a medication that dries the mouth and throat too much, which can make the soreness feel worse even if the runny nose improves.
This video gives a practical overview of symptom relief approaches people often use at home:
When to See a Doctor for Your Sore Throat
Some sore throats are straightforward. Others shouldn't be managed by guesswork.
If symptoms fit a clean allergy pattern and improve with allergen control plus over-the-counter treatment, home care is reasonable. If the picture is mixed, severe, or persistent, an exam becomes much more useful.
Red flags that need prompt evaluation
Seek medical care quickly if you have:
- Difficulty breathing or swallowing
- High fever or worsening fever
- White patches on the tonsils
- Dehydration
- A spreading rash
- Severe one-sided throat pain
- Symptoms that keep returning without a clear trigger
A sore throat with fever is not something to dismiss as “just allergies” without a closer look.
In Lanham and Prince George's County, this is especially important for patients balancing work, family responsibilities, travel requirements, or immigration-related appointments. A delayed diagnosis can create avoidable problems if the underlying issue is strep, COVID-19, reflux, or another condition that needs specific treatment.
Why an exam matters
A clinician can do what home treatment can't. They can look for tonsil exudate, assess lymph nodes, review the timeline of symptoms, and decide whether testing is needed.
For some patients, the biggest value is not more medicine. It's diagnostic clarity. That's particularly true when symptoms overlap, when English isn't a patient's first language, or when chronic conditions such as diabetes or hypertension make people more cautious about self-treating. If you're trying to decide where a same-day evaluation fits into the right level of care, this guide on when to visit urgent care can help.
Doctors may recommend prescription nasal steroids, additional testing, or a different plan entirely if the throat pain turns out not to be allergy-related. That's the trade-off. Waiting can spare you an unnecessary visit, but it can also prolong symptoms if you're treating the wrong problem.
Frequently Asked Questions about Allergy Sore Throats
Can food allergies cause a sore throat
They can, but not in the same way seasonal allergies usually do. Food allergies may cause throat itching, mouth itching, swelling, or more serious reactions. If throat symptoms happen right after eating, especially with swelling, hives, wheezing, or breathing trouble, that needs urgent attention.
How long can an allergy sore throat last
It can last much longer than an infection if exposure continues. According to GoodRx's review of allergy sore throats, an allergy-induced sore throat can last for weeks or even months as long as you're exposed to the allergen, while a viral sore throat typically resolves in 3 to 7 days. The same review notes that pollen affects 50 million Americans yearly and dust mites affect 20 million.
Do allergy shots help if allergies cause sore throat
They can for the right patient. Allergy shots don't give quick relief the way antihistamines or nasal sprays can, but they may reduce the body's overreaction over time. They're most useful when symptoms are recurrent, predictable, and not controlled well enough with allergen avoidance and standard medication.
Can a sore throat be the only allergy symptom
Yes, it can happen, especially if postnasal drip is mild and the person mainly notices throat irritation. Still, a sore throat by itself deserves a broader differential diagnosis. Dry air, reflux, infection, and voice strain can all look similar.
What usually doesn't work well
Using antibiotics without evidence of bacterial infection usually doesn't help an allergy sore throat. Neither does treating only the throat while ignoring the nose. If drainage is the driver, the plan has to target the allergy source.
If your sore throat keeps coming back, doesn't match a simple cold, or needs a clear diagnosis before work, travel, or an immigration medical exam, Maryland Primary and Urgent Care offers community-focused care in Lanham with walk-in urgent care, same-day appointments, telemedicine, and on-site testing to help you figure out what's causing your symptoms.
