A cough after the flu is very common, typically lasting 1 to 3 weeks as the airways heal, and it usually isn’t a sign of a new infection. If you’re feeling mostly better but still coughing, that pattern is often part of normal recovery, although some coughs can last longer and still improve gradually.
That’s the part many people find confusing. The fever is gone, the body aches have eased, your energy is starting to come back, and then the cough keeps showing up when you talk, laugh, lie down, or step outside into cold air. It’s frustrating, but it often reflects healing airways rather than ongoing flu.
For adults in Lanham and Prince George’s County, the most useful question isn’t “Why am I still coughing at all?” It’s “Is this cough following a normal recovery pattern, or is it time to get checked?” The answer depends on timing, symptom pattern, and whether any warning signs are starting to appear.
Table of Contents
- Your Concise Answer to the Post-Flu Cough
- Why Your Cough Lasts Longer Than The Flu
- The Typical Timeline for a Post-Flu Cough
- Effective Home and OTC Remedies for Your Cough
- Red Flags When a Lingering Cough Needs a Doctor
- How We Diagnose Persistent Coughs at Maryland Primary and Urgent Care
- Frequently Asked Questions About Post-Flu Cough
Your Concise Answer to the Post-Flu Cough
You finally feel over the flu, go back to work, and then the cough keeps showing up at night, during conversations, or the moment you step into cold air. In primary care, that pattern is common. A post-flu cough often lingers after the fever, body aches, and fatigue have already eased because the airways stay irritated longer than the rest of the body feels sick.
In practical terms, a cough that is gradually easing is usually part of normal recovery. A cough that starts intensifying again, brings new shortness of breath, chest pain, fever, or wheezing needs a closer look.
Seasonal flu is common worldwide, so this experience is common too. You are not unusual if the cough outlasts the worst part of the illness. Patients often describe the same cluster of symptoms: throat irritation, a tickle in the chest, leftover mucus, and coughing spells that flare at inconvenient times.
The goal is simple. Support healing, avoid treatment you do not need, and watch for signs that suggest something more than a routine post-viral cough. Good hydration, rest, and avoiding smoke or heavy irritants usually help. For readers also trying to understand whether frequent illnesses point to a broader issue, Yuve's immunity insights offers added background.
For patients in Lanham and Prince George's County, local access changes the experience. If your cough is hanging on or you are unsure whether it is still normal, Maryland Primary and Urgent Care can evaluate it through walk-in care or telemedicine, with on-site labs and imaging available when the history or exam suggests you need more than reassurance.
Why Your Cough Lasts Longer Than The Flu
A common office visit goes like this. The fever is gone, the body aches have passed, energy is starting to come back, but the cough still shows up during phone calls, at bedtime, or the minute you step into cold air. In primary care, that pattern usually points to airway recovery that is still in progress rather than a flu infection that is still active.
Your airways stay irritated after the infection ends
Flu can leave the lining of the throat and bronchial tubes inflamed for longer than the rest of the illness lasts. As that lining heals, it remains sensitive. Coughing is one of the ways the body responds to that irritation.
Patients usually notice this in very ordinary situations. Talking for several minutes, laughing, breathing cold outdoor air, or lying down at night can trigger coughing spells. The virus may be gone, but the airway has not fully settled.
The distinction between cough types guides treatment decisions. A gradually improving cough often needs time and symptom relief. A cough that is getting harsher, more frequent, or more painful deserves a closer look.
Mucus clearance can stay sluggish
After flu, mucus often lingers even when heavy congestion has improved. The airways may still be producing extra secretions, and the normal clearing mechanism can be less efficient for a while. That leaves people with throat clearing, a wet cough, or the sense that something is stuck in the chest.
A few practical measures help more than patients expect:
- Hydration: Fluids can thin mucus and reduce throat irritation.
- Humidity: Moist air may ease dryness that keeps the cough reflex active.
- Trigger control: Smoke, vaping, dust, strong scents, and cold air commonly keep symptoms going.
For people who are also wondering whether they tend to get sick often or recover slowly, Yuve's immunity insights add useful background on broader health factors that can affect recovery.
The cough reflex can stay oversensitive
The other piece is a cough reflex that remains turned up after the flu. Even mild irritation can set it off. That is why some people feel almost back to normal, then start coughing after a deep breath or a short laugh.
I often explain this to patients in Lanham and Prince George's County because it helps lower anxiety and improve judgment. If the story and symptoms fit a routine post-viral cough, reassurance and supportive care are often enough. If the pattern suggests pneumonia, asthma, bronchitis, or another problem, Maryland Primary and Urgent Care can evaluate it through walk-in visits or telemedicine, and we can arrange on-site labs and imaging when the exam points to something more than routine healing.
The Typical Timeline for a Post-Flu Cough
A common office visit goes like this. The fever is gone, energy is starting to come back, but the cough is still hanging on. Patients usually want to know whether that is normal or whether they are missing pneumonia, bronchitis, or something else.
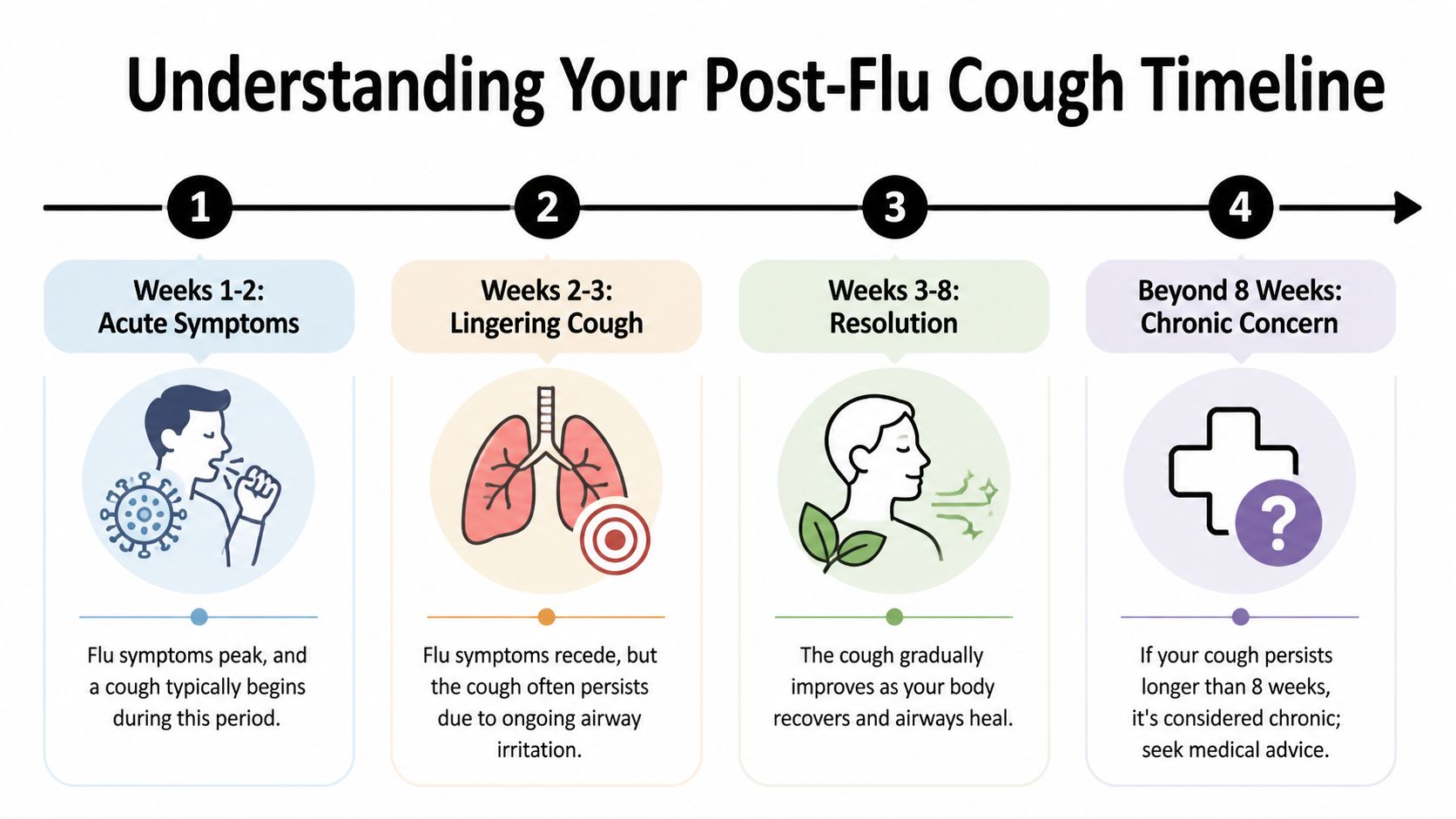
What the timeline usually looks like
For many adults, a cough after the flu settles within 1 to 3 weeks. Some people keep coughing longer, especially if the airways stay irritated after the infection clears. A cough can still fit a postinfectious pattern for up to 8 weeks, as noted earlier.
Here is the practical way to look at it:
| Phase | Time frame | What it usually means |
|---|---|---|
| Early recovery | Up to 3 weeks | Common during normal airway healing |
| Subacute cough | 3 to 8 weeks | Often still fits a post-viral cough pattern |
| Chronic cough | Beyond 8 weeks | Deserves evaluation for another cause |
The 3 to 8 week window causes the most worry. It feels like the illness should be over by then, but the cough reflex often recovers more slowly than the rest of the body.
That said, the calendar is only part of the decision.
A simple way to judge progress
The better question is whether the cough is improving, staying flat, or getting worse. A mild cough that slowly fades is very different from a cough that becomes deeper, more frequent, or starts disturbing sleep after it had been easing up.
Signs that the course is still reassuring include:
- Gradual improvement: You are coughing less often, or the coughing spells are less intense.
- Stable breathing: There is no new shortness of breath with routine activity.
- No return of systemic symptoms: Fever, shaking chills, or worsening fatigue are not coming back.
- Less chest congestion over time: Mucus may still be present, but it is trending down rather than building.
Patients in Lanham and Prince George's County often ask when to stop watching and come in. My advice is simple. If the trend is not clearly improving after a few weeks, or if the cough reaches the 8 week mark, it is reasonable to get checked at Maryland Primary and Urgent Care. We can start with a walk-in visit or telemedicine, then add on-site testing when the history or exam suggests asthma, pneumonia, sinus drainage, reflux, or another cause.
If you are trying to support recovery between visits, clean solutions for respiratory care offers practical guidance on air quality and lung comfort at home. If you also want help choosing cough products safely, especially with blood pressure medicines or other chronic conditions in the mix, on-site pharmacist counseling at Maryland Primary and Urgent Care can help you sort through the trade-offs.
Effective Home and OTC Remedies for Your Cough
Individuals typically don’t need aggressive treatment for cough after flu. They need symptom relief, patience, and realistic expectations.

What helps at home
Home care works best when it reduces irritation instead of trying to force the cough to disappear overnight.
A few measures tend to make the biggest difference:
- Drink regularly: Water, warm tea, and broth can soothe the throat and thin mucus.
- Use a humidifier: Dry indoor air often makes post-viral cough worse.
- Try honey if appropriate for you: It can coat the throat and reduce irritation.
- Sleep with your head raised: This can help if post-nasal drip is triggering nighttime cough.
- Avoid smoke and strong scents: Healing airways are easily provoked.
Some readers also like broader, non-drug approaches to supporting lung comfort at home. Clean solutions for respiratory care gives a practical overview of air quality and breathing-support habits that fit well with conservative recovery care.
If you want help choosing nonprescription products safely, especially if you also manage high blood pressure, diabetes, or other chronic conditions, on-site pharmacist counseling at Maryland Primary Care is a useful local resource.
How to think about OTC cough products
Over-the-counter options can help some people feel more comfortable, but they don’t reliably shorten the course of postinfectious cough. That distinction is important.
Systematic reviews of randomized controlled trials found no significant evidence of benefit from inhaled corticosteroids, bronchodilators, or other oral medications for postinfectious cough, and most studies showed improvement over time without pharmaceutical intervention, according to this review of treatment evidence.
That doesn’t mean every OTC product is useless. It means you should treat them as comfort tools, not cures.
Common ways people use them include:
- Cough suppressants: Sometimes helpful at night if coughing is preventing sleep.
- Expectorants: Some people prefer them when mucus feels thick.
- Lozenges: Often useful for throat irritation and frequent throat clearing.
Here’s a brief visual guide if you want to see basic self-care measures in action before buying anything else.
The trade-off is simple. Symptom relief may be worth it if you’re sleeping poorly or coughing through meetings. But if a product isn’t helping after a reasonable try, it’s usually smarter to stop chasing medications and focus on hydration, humidity, rest, and monitoring the trend.
Red Flags When a Lingering Cough Needs a Doctor
A common scenario in clinic is this: the fever is gone, body aches have eased, but the cough is still hanging on and patients start asking whether they should keep waiting or get checked. That question matters less by the sound of the cough alone and more by the pattern around it.
Normal healing versus warning signs
A post-flu cough can stay irritating for a while and still be part of recovery. What changes the picture is new breathing trouble, bleeding, pain, trouble swallowing, or a cough that is not improving at all.
| Symptom | More consistent with recovery | Signs you should get medical care |
|---|---|---|
| Cough pattern | Dry or mildly productive cough that is gradually easing | Cough that is getting worse, stays intense, or shows no improvement |
| Breathing | Brief throat or chest irritation while coughing | Shortness of breath or breathing that feels harder than expected |
| Chest symptoms | Muscle soreness from repeated coughing | Chest pain, especially if it is persistent or not clearly from muscle strain |
| Blood | No blood in mucus | Hemoptysis |
| Voice and throat | Mild temporary irritation | Hoarseness or dysphagia |
| Whole-body symptoms | Energy slowly returning | Systemic symptoms such as renewed fever, marked fatigue, or unexplained weight loss |
| Time frame | Improving during the expected recovery window | Cough lasting beyond 8 weeks |
In primary care, these are the details that push a cough out of the “watch and wait” category. Post-viral cough is often harmless, but it is also a diagnosis made after more concerning causes have been ruled out.
One practical rule helps. If you are coughing but improving overall, that is reassuring. If the cough is arriving with new problems, it deserves an exam.
If you are unsure how urgent your symptoms are, this guide on when to visit urgent care can help you decide.
When persistent cough points to something else
Sometimes the flu starts the irritation, but another condition keeps the cough going. In practice, I think about asthma flare, pneumonia, sinus drainage, reflux, medication side effects, and sleep-disordered breathing, depending on the history.
Sleep apnea can be part of that picture, especially when the cough lingers alongside loud snoring, daytime sleepiness, morning headaches, or reflux symptoms. Those clues do not prove the diagnosis, but they do change the next step. A patient in Lanham or elsewhere in Prince George's County does not need to guess through that alone. Maryland Primary and Urgent Care can evaluate a persistent cough with walk-in access, telemedicine when appropriate, and on-site labs or imaging if the symptoms suggest something more than routine recovery.
Clues that deserve closer attention include:
- Loud snoring
- Daytime fatigue
- Morning headaches
- A cough that does not settle when reflux, poor sleep, or nighttime symptoms are also present
For readers using oxygen support or helping a family member with chronic lung disease, this practical guide for oxygen devices explains how those devices fit into broader respiratory care. It does not replace a medical evaluation, but it can help you ask better questions at the visit.
How We Diagnose Persistent Coughs at Maryland Primary and Urgent Care
When a cough after flu doesn’t follow the expected path, the goal is to sort out whether this is still post-viral healing or whether another diagnosis needs attention.

What the visit usually includes
A good evaluation starts with basics done well. That means listening to the timeline, checking whether the cough is dry or productive, reviewing fever history, and asking what triggers the cough now that the flu itself has mostly passed.
In clinic, the workup may include:
- A focused physical exam: Lungs, oxygenation, throat, nasal drainage, and signs of breathing strain.
- On-site labs when appropriate: Helpful when symptoms raise concern for ongoing infection or overlap with another illness.
- Imaging when indicated: Chest imaging can help rule out pneumonia or other lower respiratory problems.
- Review of underlying conditions: Asthma, reflux, smoking history, and sleep symptoms can change the picture.
If infectious symptoms are still part of the concern, PCR testing in Maryland and infectious disease evaluation can be part of the diagnostic pathway.
The most useful visit isn’t the one that automatically gives medication. It’s the one that clarifies what kind of cough you actually have.
Why local access matters
Convenience changes outcomes in real life. A patient with a nagging cough may put off care if getting evaluated means a long delay, a separate imaging appointment, and no follow-up plan.
That’s where integrated local care helps. Walk-in urgent care works when symptoms feel more immediate. Same-day primary care helps when the issue is persistent but stable. Telemedicine follow-up makes sense when the main need is symptom review, medication guidance, or checking whether the cough is trending in the right direction.
For more complex cases, added services matter. A persistent cough can overlap with sleep-disordered breathing, reflux, or chronic medical conditions that don’t get sorted out in a rushed, one-size-fits-all visit. Having access to on-site diagnostics and coordinated follow-up makes it easier to move from “I’m still coughing” to an actual explanation.
Frequently Asked Questions About Post-Flu Cough
Is a cough after flu still contagious
A lingering cough often comes from irritated airways after the infection has already passed. By itself, that does not confirm you are still contagious.
The full symptom pattern matters more. New fever, renewed body aches, worsening congestion, or feeling sick again deserves another evaluation, especially if symptoms had started to improve and then turned back in the wrong direction.
Why is the cough worse at night
Nighttime cough is one of the most common complaints I hear after flu. Lying flat can increase throat irritation, post-nasal drainage, and reflux. Bedrooms also tend to be dry, which can keep a cough cycle going.
Simple changes can help. Raise your head slightly, keep the room from getting too dry, and avoid eating right before bed if reflux might be part of the problem.
Should I ask for antibiotics
Antibiotics are usually not the right treatment for a routine post-flu cough. They do not treat the lingering airway inflammation that often follows a viral illness.
They do have a role when the exam points to something else, such as pneumonia, a sinus infection with bacterial features, or another complication. The trade-off is straightforward. Unnecessary antibiotics add side effects and do not speed recovery.
Is dry cough better than wet cough
Dry versus wet does not reliably tell you which cough is more serious. A dry cough often fits post-viral airway sensitivity. A wetter cough can happen with mucus, drainage from the nose and sinuses, or irritation lower in the chest.
What matters more is the trend. A cough that is gradually easing is less concerning than one that is getting stronger, disturbing sleep every night, or coming with shortness of breath.
When does a post-flu cough become chronic
Once a cough lasts longer than 8 weeks, it falls into the chronic cough category and deserves a broader evaluation, as noted earlier.
At that point, the question often shifts from "Is this still from the flu?" to "Did the flu uncover something else?" Common possibilities include asthma, reflux, smoking-related airway disease, medication side effects, or ongoing upper-airway irritation.
Can the flu uncover another health problem
Yes. Flu can bring attention to a problem that was already present but mild enough to ignore before the illness. I commonly see coughs that end up being tied to asthma, reflux, allergies, or poor sleep related to breathing issues.
That is why repeated guesswork is rarely the best plan once a cough stops following a normal recovery pattern.
Does everyone with a long cough need medication
No. Some patients improve with time, fluids, avoiding smoke or strong irritants, and getting better sleep. Others need an inhaler, reflux treatment, or treatment aimed at nasal drainage. The right answer depends on the cause.
The goal of a visit is not only to leave with a prescription. The goal is to figure out whether your cough is still part of recovery or whether it needs a different diagnosis and treatment plan.
If your cough after flu is not improving, or it is keeping you up at night, causing chest discomfort, or making you short of breath, Maryland Primary and Urgent Care gives patients in Lanham and Prince George's County a practical next step. You can use walk-in urgent care for more immediate concerns, book a same-day primary care visit for a persistent but stable cough, or choose telemedicine for follow-up and symptom review. On-site diagnostics can help speed up the workup when the cough needs more than reassurance.
